Women’s experiences with the health service provision for medical abortions in Norway
They feel like a burden on resources and have a need for care and real co-determination.
Background: Most pregnancy terminations in Norway are carried out as medical abortions, either in a hospital or in the patient’s home. Abortions must be carried out according to the same standards as other health services, but existing knowledge leads us to question whether this is actually being done.
Objective: The objective of this study was to shed light on women’s experiences with the health service provision for medical abortions in Norway.
Method: The study had an exploratory-descriptive design, and involved individual interviews with 24 women who had undergone a medical abortion at home before the end of the twelfth week of pregnancy. The data were analysed using systematic text condensation.
Results: The women mostly reported negative experiences with healthcare personnel and the health service. The main findings relate to the women’s perceptions of themselves as a burden on resources and not deserving of care, their encounters with a standardised, one-dimensional service that focuses on physical aspects rather than a person-centred approach, and their perceived lack of freedom of choice, co-determination and preparedness.
Conclusion: The women found that there was limited opportunity to talk about their abortion choices. They also considered there to be insufficient information and access, and felt there was no individual approach when they felt uneasy or there were unexpected developments. Other experiences included being met with an attitude of remoteness and a lack of respect on the part of healthcare personnel, as well as a feeling of loneliness. Access to personnel with in-depth knowledge of the abortion process, for example midwives, can strengthen the service provision and ensure professional reliability.
Introduction
Access to abortion is an essential part of the service provision within sexual and reproductive health, and it must meet the same standards as other health services. In Norway, women have the right to a self-determined abortion up to the twelfth week of pregnancy. Medical abortions, i.e. pregnancies terminated using medication as opposed to surgery, were introduced in 1998. In 2021, 10 349 out of a total of 10 841 abortions were carried out using this method (1).
The World Health Organisation (WHO) (2) has estimated that half of all abortions worldwide are carried out in the least safe or dangerous conditions. Unsafe abortions are pregnancies that are terminated by people who do not have the necessary skills, and/or occur in an environment that does not conform to minimum medical standards.
Medical abortions normally involve the woman taking a tablet containing the active ingredient mifepristone at a gynaecological clinic after the pregnancy has been confirmed. Two days later, the woman takes a tablet called misoprostol, which causes the uterus to contract and the foetus to pass (3).
The Norwegian abortion register does not have statistics on the proportion of women who carry out the second part of the abortion at home. According to Helsenorge’s information pages, women in Norway must be given the option of a surgical or medical abortion (3). If the woman chooses a medical abortion, she must also be able to choose whether she wants to carry it out in hospital or at home.
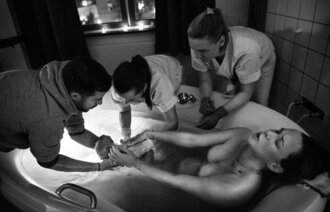
This study shines a spotlight on medical abortions at home. The practice for carrying out abortions at home is standard throughout Norway. The woman must be healthy, and some hospitals set a lower age limit of 18. The women are advised to have someone with them during the abortion. At some hospitals, a registered nurse (RN) will call the woman after a few days to find out how things went. After four weeks, it is recommended that the woman takes a pregnancy test to confirm that the abortion was successful (4).
Medical abortions must be carried out in a respectful and responsible manner based on openness, understanding and equality, thereby protecting the individual’s right to self-determination (3, 4). Recent research shows that on a global scale, health services fail to provide a person-centred approach to pregnancy termination. Many women find having an abortion a lonely and challenging process with existential dimensions (5–7).
The women may feel ambivalence, and some are still unsure of their decision when they arrive at the gynaecology clinic (3, 6). A meta-synthesis of six qualitative studies indicates that healthcare personnel take care of women’s physical health after an abortion, but that little or no attention is paid to their psychological and emotional needs (8). The option of carrying out a medical abortion at home can give women a sense of autonomy, depending on what information is provided and their perceptions of the interaction with the healthcare personnel (9–11).
Deeply rooted social stigmas, institutional limitations, and laws and regulations can all be barriers to a person-centred approach to pregnancy termination (12). Stigmatisation often leads women to keep their abortion secret, often for many years (13–15). Negative attitudes to abortion in general can be seen both within and outside the health service and can impact on the women’s experience of the pregnancy termination process (9, 13).
Good reproductive and sexual health is a goal in public health work, with a view to promoting welfare and counteracting social inequality. Society has an obligation to prevent unwanted pregnancies (5). Women who choose to have an abortion must be able to have it as quickly as they want, using the best method based on medical criteria and the women’s own wishes (4). A person-centred approach is a key dimension in the quality of health services, where the care they receive encompasses the patients’ personal perspectives, needs and values.
Objective of the study
The objective of this study was to shed light on women’s experiences with the health service provision for medical abortions in Norway.
Method
The study had an exploratory-descriptive design (16) and involved individual interviews (17). The study is part of a larger research project that explores various aspects of women’s experiences with medical abortions, such as guilt, shame and a lack of emotional availability (5, 9).
Sample and data collection
The sample consisted of 24 women. The inclusion criterion were women who had undergone a medical abortion before the end of the twelfth week of pregnancy. We posted an announcement on Facebook in our search for participants, providing a link to the university where we are employed. Within a day, 27 women had expressed an interest in participating, and the advertisement was subsequently removed.
After receiving written informed consent from the informants by email, they were distributed among six researchers in the group, who conducted the interviews from October 2019 to January 2020. Three women declined to participate when we contacted them to arrange an interview date.
We interviewed two informants via Zoom (18) due to the distances involved. The others were interviewed at a location of their choice, in private settings, often at nearby colleges or universities or in their own home. We used an interview guide with the following open-ended questions:
Introductory question: ‘Can you tell me about the abortion you had some time ago?’
Additionally: ‘What was your experience of having a medical abortion at home? How did you find the interaction with the health service during the process? What follow-up were you offered after the abortion?’
The informants were encouraged to talk about specific experiences related to the health care they received in connection with their medical abortion. The women spoke freely, and we requested further information when there was a need for elaboration and clarification.
The interviews lasted from 19 to 71 minutes, with an average of 47 minutes. We made audio recordings during the interviews and transcribed them verbatim. The total scope of the data material was approximately 360 pages of text.
Analysis
We analysed the data using systematic text condensation (STC), a four-step strategy for cross-sectional thematic analysis of qualitative written data material (19). In the first step of the analysis, all the interviews were read to get an impression of preliminary themes as a basis for further analysis.
We then identified meaning units in the data material that related to the informants’ experiences with the health service. These were systematically coded into groups dealing with the same phenomenon, and then sorted into subgroups. The content of each subgroup was condensed into an artificial quotation that reiterates and summarises the content of the subgroup.
Finally, we used the condensates to develop an analytical text consisting of three themes. The first analysis was performed by two of the authors (AL and BMS). All the authors then discussed the analysis before reaching a consensus. We are from different disciplines in the health service, i.e. midwife, public health nurse, mental health worker and psychologist.
Ethical considerations
We submitted the study to the Norwegian Centre for Research Data (NSD) (reference number 22708). The Regional Committee for Medical and Health Research Ethics (REC) determined that the study is outside the remit of the Health Research Act (reference number 36616).
The participants received oral and written information about the study before the interviews, and signed an informed consent form. They were informed that they could withdraw from the study at any time without any repercussions, and that all the data they had provided would be deleted before the analysis began.
Results
The informants were women aged 24–45, from seven counties in Norway spread from north to south. The women had had a medical abortion between 2008 and 2019, most of which had taken place in the past four years.
The women mainly reported negative experiences with healthcare personnel and the health service in general. Based on the data analysis, we can categorise the women’s experiences in the following themes: ‘Treated like a second-class citizen’, ‘A standardised approach’ and ‘Duped by the health service’.
Treated like a second-class citizen
Informants with previous patient experiences felt like a burden on resources. They did not receive the same care from the health service that they had experienced previously in other contexts.
Some women were subjected to comments such as ‘Don’t you know how you get pregnant?’, or what one informant described as a ‘damning silence’. Others felt that hospital personnel had a judgemental attitude. They were doing something that was ‘completely legal’, but which they found to have a great deal of shame attached to it:
‘No one was rude exactly, but they didn’t go out of their way to make me feel better. But it’s difficult for me to say whether that was to do with how she treated me or whether it was my own feeling of shame, and that I myself felt that I didn’t deserve care.’ (informant 23)
The women felt that few people cared about how they felt. When they tried to talk about the difficult choice, some felt rejected and were told ‘This is your choice and you don’t need to talk to us about it’, or they were not given more time to consider the abortion decision:
‘When I arrived to take the tablet, they said that when you take it, all life ends. So I said: “No, we’ll think have a think about it”, and she replied: “You don’t have any more time to think about it now”, and I said: “Okay, yes, no, then I’ll take the tablet here.” It was pretty brutal. I wasn’t strong enough to say stop.’ (informant 22)
The women described a situation where they were shown little empathy or care from the healthcare personnel throughout the abortion process. Once they had taken the tablet that ends the life of the foetus, they were left to their own devices. They were given the medication to pass the foetus. Some were given painkillers. Then they went home, and the process was underway. Most women received no follow-up after the abortion:
‘When you have an operation, they call you after three days and ask how you’re doing and stuff like that. So you feel kind of looked after. I wish it was the same here.’ (informant 10)
A standardised and mechanical approach
The women considered the healthcare personnel’s approach to the medical abortion to be standardised and mechanical, and in terms of examination and information it was ‘a bit like an assembly line’. The women described the focus as being on quick physical examinations and practical procedures, with little dialogue. For some, it was fine because it meant they didn’t have to deal with their thoughts and emotions. The informants did not feel that they were seen and respected by the healthcare personnel:
‘If you only got some confirmation that it’s your choice, and it’s perfectly okay that you’ve made this choice. And I think that’s really important for how you process it all afterwards.’ (informant 4)
Several of the women were not asked if they wanted to look at the ultrasound images of the foetus. Those who spoke up felt that their wishes were not being met. Some of the women were shown the images and the healthcare personnel talked about what they were looking at in the images even when the woman did not want this information. Several women who had asked to see the images were not allowed to do so:
‘I asked, but they said, “No, you can't” …. I was actually a bit in doubt as to whether I should have an abortion, so if I had been able to see the images, it might have been different.’ (informant 6)
Several women found that there was no room for dialogue. The healthcare personnel gave the impression of knowing what was in the women’s best interests. Some women felt inferior and were unable to assert their needs. Several were still in doubt about their decision when they arrived at the hospital, but there was no one to talk to. One woman said she did not make a conscious choice, that it just happened. Another thought that if she had been treated with understanding and had been able to talk about the decision, it might have been different: ‘And it’s quite difficult to deal with afterwards.’
For some, it was good not to have to talk about the abortion and to be able to put it behind them:
‘In a way, I’m kind of done with the process, so if I have to go in again and get a follow-up, then maybe you start to feel that bad conscience again... in a way.’ (informant 3)
Several women said that abortion is not something they talk about with friends and family, because the subject was taboo and shameful for those who have been through it:
‘There probably hasn't been a day since when I haven’t… uh… thought about it…. So really, they should offer you a follow-up conversation afterwards as well... about how it went.’ (informant 6)
Duped by the health service
For some informants, contacting the hospital was uncomplicated, while for others, it presented challenges. Some received help from their local midwife to book an appointment at the hospital, and others went through their GP or contacted the hospital directly. Some did not know how many weeks they had been pregnant. They found that this was not taken into account when they booked an appointment, and felt de-prioritised:
‘So then I called the hospital again, and I was allowed to come the next day. But it was a bit like: “Yes, but you’re at the bottom of the priority list, so you’ll just need to sit and wait. You may need to wait all day. In the waiting room. But that’s the way it is.” ’ (informant 8)
Only a small number of the women were given the choice between carrying out the abortion at home or in hospital. Those who were given this choice felt they had been listened to:
‘The offer was there, but I thought it would be nice to go home. I don't know if that’s usual, or if you just get sent home. I felt they really listened to me. I think it’s important to be given the choice of whether you want to be at home or in hospital.’ (informant 8)
Some women found that they consented to a medical abortion at home on a flawed basis. Others felt they were not given a real choice. The information they received about the home abortion gave the impression that it was an uncomplicated process. Others thought that the only difference between an abortion at home and in the hospital was where they took the remainder of the tablets. It was tempting to be at home in familiar surroundings. Very few felt adequately prepared:
‘She asked me, “Do you want to have the abortion in the hospital, or at home?” So I asked her, “What’s the difference?” I had no idea what it might be, and she didn't explain it to me either, she just said, “You’ll get some tablets, some vaginal tablets, and then you can decide for yourself whether you want to take them here or at home.” ’ (informant 12)
The information they received about what was going to happen during the abortion process contrasted strongly to what most of the women experienced at home alone or together with their family, boyfriend or friend:
‘No one prepared me for how intensely painful it was. It’s the worst thing that’s ever happened to me, it’s much worse than giving birth. I remember thinking that this can't be normal, because if it had been normal, you wouldn't have been sent home to do it.’ (informant 23)
Several informants were left with a feeling of having been deceived, and would advise others against a medical abortion at home:
‘When I think about medical abortions, I wonder: “Who is this benefitting the most? Is it the health service, or is it the patient?” It was presented to me as if this is how it happens, and not as a choice.’ (informant 18)
The women found the information they received prior to the abortion difficult to understand. They felt alone and insecure, and lacked safe surroundings and contact with a specialist. They felt that no one cared about how much pain they were in, and how scared they were:
‘I can’t think of anything else that causes such severe pain, which you’re asked to deal with at home alone.’ (informant 6)
Several women were afraid of dying during the treatment. Although most had followed the recommendation to have someone with them, they felt that the situation was unsafe and unacceptable. The person helping them (not a healthcare professional) had no knowledge of what constituted a normal abortion process. Help and support were therefore limited. Many of the helpers also found the situation traumatic:
‘To send someone home and say that you just have to manage this on your own in your own home, that’s .... It’ll all be fine. They don't even say that, they just send you home with a tablet and say “Go home now and follow the instructions.”. I think it’s irresponsible, just sending someone home. I don’t think anyone should be alone in a situation like that, with only an unqualified person present. There should definitely be qualified staff in attendance. It should be in a hospital. I think this practice is misogynistic, really, in lots of ways.’ (informant 20)
Discussion
The objective of this study was to shed light on women’s experiences with the health service provision for medical abortions at home. The women who were interviewed felt alone in making their choice and also that they were left to their own devices during the actual abortion. A medical abortion at home is regarded by medical professionals as an effective and acceptable method of pregnancy termination (20).
According to Kjelsvik et al. (6), women who wish to terminate their pregnancy expect to be treated with respect by the health service. Aiken et al. (21) describe how women seeking an abortion are treated with a lack of understanding, and counselling and support are rarely offered.
Findings from our study show that women were made to feel that they were a burden on the health service. They interpreted both verbal and non-verbal communication to mean that the healthcare personnel felt they should not have become pregnant in the first place.
It is conceivable that women seeking abortions are particularly sensitive to how they are treated in this vulnerable situation. Healthcare personnel are subject to a special requirement to show respect and understanding for the women’s situation. The results of this study provide a basis for asking questions about whether the quality of the health service provision is good enough, and whether women’s patient rights are adequately protected.
In the study by Makenzius et al. (22), the need for a continuous evaluation of the abortion provision is emphasised. Furthermore, Mariutti et al. (23) conclude that there is a need to create an environment in which more attention is paid to women who need to discuss their situation and explore their often mixed emotions about the abortion.
Lack of a person-centred approach
In Norway, it is a guiding principle that women have bodily autonomy, as provided for in the Abortion Act. Women’s right to information, co-determination and self-determination is formulated in the wording of the Act (24). According to Kjelsvik et al. (6), the health service may be overlooking the existential questions that a decision about abortion can raise.
Kjelsvik and Gjengedal (25) revealed that 10–20 per cent were still unsure whether they should have an abortion when they arrived for the initial procedure. Consultations in which healthcare personnel are open to discussing the issue could help create a sense of empathy and give the women new perspectives without compromising their self-determination. Such consultations can strengthen women’s ability to make autonomous and informed choices (26, 27).
The informants in our study found that the healthcare personnel’s focus tended to be on physical aspects and examinations, and that they followed standardised procedures rather than taking a person-centred approach. The person-centred approach seems to be missing in relation to women considering an abortion. A person-centred approach is about empowerment, equality, respect and protecting the individual’s needs (28).
Midwives should be included in the health service provision
A British study describes how the responsibility for providing medical abortions has been moved from the specialist health service to primary health care (29). The intention is to give the women local access to professionals who can talk to them and answer their questions throughout the abortion process. Users’ evaluations of this have been positive (29).
Providing for medical abortions in primary health care may make the adoption of a person-centred approach in the treatment process more straightforward. In this context, it is opportune to suggest that midwives should be included as part of this service provision. Midwives work in the specialist health service and in primary health care and are knowledgeable about all aspects of women’s reproductive health, including the abortion process (30). A midwife can be good support for women who want contact before, during and after the pregnancy termination.
The RNs must be able to communicate well
The informants in the study found that the oral and written information they received about what to expect was in strong contrast to their experience of abortion in their own home. Aamlid et al. (9) describe in their study how the information is perceived as insufficient, to the extent that many women are fearful and unprepared for severe pain and heavy bleeding during the process. A study from Sweden also shows that many women receive insufficient information and have heavier bleeding and more pain than expected (13).
This is consistent with our findings. Many reported heavy, prolonged bleeding and pain. Several informants claimed that they would never have subjected themselves to a medical abortion at home if they had understood what was involved. Women must be free to choose a surgical or medical abortion as long as it is clinically safe. They must be given the choice of whether they want the abortion to take place at home or in hospital (3).
Few of the study’s informants were given a choice about where the medical abortion would take place, and none were given a choice about the method of abortion. This does not sufficiently allow for informed decisions as required by law (24).
The overall results from our study give reason to assert that healthcare personnel, mainly RNs, who carry out abortion-related work, should have good communication skills. It can be a difficult balancing act for female nurses who are ambivalent about pregnancy termination, and they must have respect for women's autonomy (6). Good communication is nevertheless crucial to protecting women’s rights and experience of being seen, heard and taken seriously.
Strengths and limitations of the study
Individual interviews were well suited to exploring the informants’ experiences with a medical abortion. Open-ended interview questions helped the informants talk freely about their experiences, and this provided rich data.
As with qualitative study designs in general, our results cannot be generalised to the entire population as a relatively small sample cannot be considered representative. Advertising on the social media channel Facebook enabled us to reach a large number of people within a short period of time, and it is purely random who sees such an advertisement within the given timeframe.
Such a random selection process can reduce the risk of bias and thus strengthen the validity of the results. We cannot, however, rule out the possibility of bias in the sample. Potentially, a preponderance of the women who wanted to participate may have had negative experiences with a home abortion or been critical of the follow-up by the health service. Some experiences that are open to criticism date as far back as 2008. There is a risk that it is the negative experiences that women remember best, see Bierbrauer et al. (31).
Our results will nevertheless be transferable to other women who have a medical abortion at home in a similar socio-cultural context. It is also a strength that the informants are geographically dispersed throughout Norway and have received health care from all four different health authorities.
Conclusion
The women in our study found that the health service provides a standardised abortion process where the emphasis is on the physical aspects of the abortion. Few informants were given the opportunity to choose the abortion method or decide where it should take place.
The study shows that there is little provision for discussing abortion choices, and that where this option exists, there is insufficient information and a lack of an individual approach and of access to help in the event of psychological reactions and/or an unexpected course of events.
Women who sought an abortion found that the contact with the health service was a barrier to seeking help. Many experienced being met with an attitude of remoteness and a lack of respect by healthcare personnel, as well as a feeling of loneliness. Pregnancy termination can be made safer through access to personnel with in-depth knowledge of the abortion process, for example midwives.
The authors declare no conflicts of interest.
References
1. Akerkar RR, Askeland OM, Faugstad LA, Halvorsen GS, Heiberg-Andersen R, Hornæs MT, et al. Abortregisteret. Rapport om svangerskapsavbrot 2021. Oslo: Folkehelseinstituttet; 2022. Report 2022. Available at: https://www.fhi.no/contentassets/029843d081ce4ae3bddd3a65b17915ae/rapport-om-svangerskapsavbrot-2021-1.pdf (downloaded 15.08.2022).
2. World's Health Organization (WHO). Preventing unsafe abortion: evidence brief. Genève: WHO; 2019.
3. Helsenorge. Abortmetoder. Helsenorge; 2022. Available at: https://www.helsenorge.no/sok/?q=abort (downloaded 15.06.2022).
4. Helsedirektoratet. Handlingsplan – Forebygging av uønskede svangerskap og abort 2010–2015 – Statusrapport 2012. Oslo: Helsedirektoratet; 2012. Available at: https://www.helsedirektoratet.no/tema/abort (downloaded 15.06.2022).
5. Røseth I, Sommerseth E, Lyberg A, Sandvik BM, Dahl B. No one needs to know! Medical abortion: Secrecy, shame, and emotional distancing. Health Care for Women International. 07.07.2022. DOI: 10.1080/07399332.2022.2090565
6. Kjelsvik M, Sekse RJT, Moi AL, Aasen EM, Chesla CA, Gjengedal E. Women's experiences when unsure about whether or not to have an abortion in the first trimester. Health Care Women Int. 2018;39(7):784–807. DOI: 10.1080/07399332.2018.1465945
7. Georgsson S, Krautmeyer S, Sundqvist E, Carlsson T. Abortion-related worries, fears and preparedness: a Swedish web-based exploratory and retrospective qualitative study. Eur J Contracept Reprod Health Care. 2019;24(5):380–9. DOI: 10.1080/13625187.2019.1647334
8. Petersen MN, Jessen-Winge C, Møbjerg ACM. Scandinavian women's experiences with abortions on request: a systematic review. JBI Evidence Synthesis. 2018;16(7):1537–63. DOI: 10.11124/JBISRIR-2017-003344
9. Aamlid IB, Dahl B, Sommerseth E. Women’s experiences with information before medication abortion at home, support during the process and follow-up procedures – a qualitative study. Sexual & Reproductive Healthcare. 2021;27:100582. DOI: 10.1016/j.srhc.2020.100582
10. Kero A, Wulff M, Lalos A. Home abortion implies radical changes for women. Eur J Contracept Reprod Health Care. 2009;14(5):324–33. DOI: 10.3109/13625180903128609
11. Makenzius M, Tyden T, Darj E, Larsson M. Sweden has the highest abortion rate among the Nordic countries. Unwanted pregnancies should be seen in a holistic perspective–individuals, health care, community. Läkartidningen. 2013;110(38):1658–61. PMID: 24199440
12. Altshuler AL, Whaley NS. The patient perspective: perceptions of the quality of the abortion experience. Curr Opin Obstet Gynecol. 2018;30(6):407–13. DOI: 10.1097/GCO.0000000000000492
13. Hedqvist M, Brolin L, Tyden T, Larsson M. Women's experiences of having an early medical abortion at home. Sex Reprod Healthc. 2016;9:48–54. DOI: 10.1016/j.srhc.2016.07.003
14. Hanschmidt F, Linde K, Hilbert A, Riedel‐Heller SG, Kersting A. Abortion stigma: a systematic review. Perspectives on Sexual and Reproductive Health. 2016;48(4):169–77. DOI: 10.1363/48e8516
15. Maxwell KJ, Hoggart L, Bloomer F, Rowlands S, Purcell C. Normalising abortion: what role can health professionals play? BMJ Sex. 2021;47(1):32–6. DOI: 10.1136/bmjsrh-2019-200480
16. Polit DF, Beck CT. Nursing research: generating and assessing evidence for nursing practice. 11th ed. Philadelphia: Lippincott Williams & Wilkins; 2021.
17. Brinkmann S, Kvale S. Doing interviews. 2nd ed. London: SAGE Publications; 2017.
18. Zoom Video Communications. Available at: https://zoom.us (downloaded 11.08.2022).
19. Malterud K. Kvalitativ metasyntese som forskningsmetode i medisin og helsefag. Oslo: Universitetsforlaget; 2017.
20. Løkeland M. Medikamentell abort i 9.–12. svangerskapsveke. Tidsskrift for Den norske legeforening. 17.06.2010. DOI: 10.4045/tidsskr.10.0561
21. Aiken A, Gomperts R, Trussell J. Experiences and characteristics of women seeking and completing at-home medical termination of pregnancy through online telemedicine in Ireland and Northern Ireland: a population-based analysis. Bjog. 2017;124(8):1208–15. DOI: 10.1111/1471-0528.14401
22. Makenzius M, Tyden T, Darj E, Larsson M. Women and men's satisfaction with care related to induced abortion. European Journal of Contraception and Reproductive Health Care. 2012;17(4):260–9. DOI: 10.3109/13625187.2012.688149
23. Mariutti MG, Almeida AM, Panobianco MS. Nursing care according to women in abortion situations. Revista Latino-Americana de Enfermagem (RLAE). 2007;15(1):20–6. DOI: 10.1590/s0104-11692007000100004
24. Lov 13. juni 1975 nr. 50 om svangerskapsavbrudd (abortloven). Available at: https://lovdata.no/dokument/NL/lov/1975-06-13-50/§11 (downloaded 15.06.2022).
25. Kjelsvik M, Gjengedal E. First‐time pregnant women’s experience of the decision‐making process related to completing or terminating pregnancy – a phenomenological study. Scandinavian Journal of Caring Sciences. 2011;25(1):169–75. DOI: 10.1111/j.1471-6712.2010.00807.x
26. Makenzius M, Tydén T, Darj E, Larsson M. Autonomy and dependence – experiences of home abortion, contraception and prevention. Scandinavian Journal of Caring Sciences. 2013;27(3):569–79. DOI: 10.1111/j.1471-6712.2012.01068.x
27. Kjelsvik M, Sekse RJT, Moi AL, Aasen EM, Nortvedt P, Gjengedal E. Beyond autonomy and care: experiences of ambivalent abortion seekers. Nursing Ethics. 2019;26(7–8):2135–46. DOI: 10.1177/0969733018819128
28. McCormack B, van Dulmen S, Eide H, Skovdahl K, Eide T. Person‐centredness in healthcare policy, practice and research. Person‐Centred Healthcare Research. Wiley Online Library. 2017:3–17. DOI: 10.1002/9781119099635
29. Cameron ST, Glasier A, Dewart H, Johnstone A, Burnside A. Telephone follow-up and self-performed urine pregnancy testing after early medical abortion: a service evaluation. Contraception. 2012;86(1):67–73. DOI: 10.1016/j.contraception.2011.11.010
30. Utdannings- og forskningsdepartementet. Rammeplan med forskrift for jordmorutdanning. Oslo: Utdannings- og forskningsdepartementet; 2005. Available at: https://www.regjeringen.no/globalassets/upload/kilde/kd/pla/2006/0002/ddd/pdfv/269373-rammeplan_for_jordmorutdanning_05.pdf (downloaded 15.06.2022).
31. Bierbrauer A, Fellner MC, Heinen R, Wolf OT, Axmacher N. The memory trace of a stressful episode. Current Biology. 2021;31(23):5204–13. DOI: 10.1016/j.cub.2021.09.044
























Comments