The organisation of community nursing services may impact negatively on safety and the quality of care
Some municipalities gave considerably more prominence to finances and day-to-day operations than safe and secure patient experiences.
Background: Norway’s community nursing service is the country’s largest primary care provider, and user numbers are increasing. The way that the community nursing service is organised may contribute to improving or reducing safety and the quality of care. The Government favours an evidence-based organisational model.
Objective: This study was conducted in order to increase our knowledge of how municipal decision-makers justify their choices, and how they describe and accentuate quality, patient safety and health promotion with respect to the organisation of the community nursing service.
Method: The study is based on a comparative case study of two Norwegian municipalities. We gathered data by conducting focus group interviews with local councillors in each of the municipalities and individual interviews with the respective heads of municipal healthcare services. We also retrieved a number of municipal documents. We subjected the material to an inductive content analysis and compared the data obtained from the two municipalities.
Results: Formal recommendations put forward by the municipal administration have a significant impact on how the community nursing service is organised in each municipality, while evidence-based knowledge and health promotion are of limited importance. Concerns for quality and safety have a moderate impact in one of the municipalities, while they have little impact in the other. There appears to be considerable distance between the levels of decision-maker and patient.
Conclusion: The study shows that the organisation of community nursing services is complex and fragmented, and there is reason to ask whether the organisation of services allows for fulfilment of legal requirements pertaining to quality and safety.
Norway’s community nursing service is the country’s largest primary care provider, and user numbers are increasing (1, 2). In Norway, it is the local authorities that are responsible for organising the municipal community nursing services. Organisational choices are made locally by elected local councillors in partnership with the municipal administration.
Decisions may be made on the basis of an instrumental rationality in which the best solution is chosen based on clear objectives and available information about all conceivable ways of achieving these objectives. Decisions may also be made on the basis of a communicative rationality, in which the actors involved in the decision-making process have different objectives and values, and decisions are based on a negotiated consensus (3).
Municipal organisation
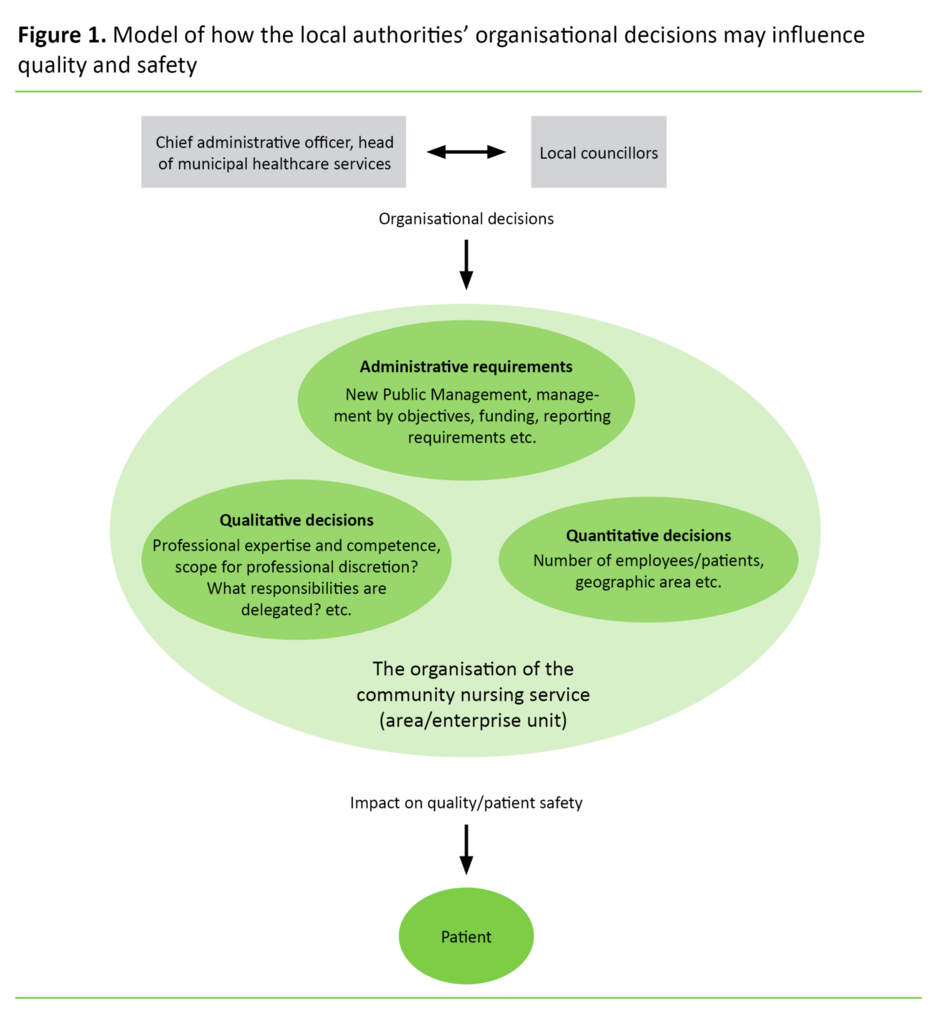
The way that Norway’s municipalities organise their community nursing services affects the quality of service as well as patient safety. In this article, high-quality services are conceptualised as effective, safe and co-ordinated services that ensure user influence through user involvement, and provide continuity (4). The choice of organisational model for the community nursing service is made by decision-makers like local councillors and the municipal administration. Their choices influence three different factors:
- The number of staff that any one patient will need to relate to,
- the professional expertise and competence available among staff, and
- (external) administrative requirements and expectations that may interact with or follow from decisions made.
According to the Norwegian Government, patients are often required to relate to many unfamiliar members of staff within their own personal space. This can affect the patients’ continuity of care, dignity, sense of security and level of safety (5). The requirements imposed by decision-makers with respect to the professional expertise and competence of those who provide the care, can also considerably affect quality and safety levels (6).
One example is competence levels in rehabilitation, where the attention is directed towards what is important for the patient (7). It is also important that community nurses are given scope to use their professional discretion. The provision of nursing care is contingent on room for negotiation and the opportunity to accommodate genuine service user involvement (8).
New Public Management
Decision-makers also influence the administrative requirements imposed on the community nursing service, as well as the nature and extent of reporting to the management by staff. Many Norwegian municipalities introduced instruments based on New Public Management approaches such as management by objectives and a purchaser–provider model (9).
A purchaser–provider model defines the need for care through a decision made by parties (the purchaser) other than those who provide the patient care. Studies suggest that the model may lead to increased bureaucracy through standardisation, regulatory control and paperwork (10), which in effect can reduce the opportunity to provide service user involvement (11). Figure 1 shows how the three above factors influence the quality of the care provided as well as patient safety.
Objective
There is limited knowledge available about the decision-makers’ reasons for choosing particular organisational models and what factors they take into consideration in this connection. Our study set out to gain more knowledge about how local authority decision-makers justify their decisions and how the factors of quality, patient safety and health promotion are described and accentuated with respect to the organisation of community nursing services. The study deals with the following research question:
- How do local councillors and the heads of municipal healthcare services describe good quality and patient safety in relation to community nursing, and how does this impact on the current organisation of these services?
Method
The study was based on a comparative case study (12) of two municipalities (‘municipality 1 and 2’) carried out in the period 2015–2016. A case study may be defined as empirical research that uses various data collection methods to investigate a contemporary phenomenon (the case) in its real-life context, particularly when the boundaries between context and phenomenon are not clearly evident (12).
The two municipalities were selected on the basis of their co-location within the same region and due to the fact that their models of local government are the same, although they differ in terms of size and organisational model. Both municipalities are governed by an executive council according to the alderman model. Municipality 1 is roughly five times larger than municipality 2 in terms of population. Furthermore, both municipalities have implemented a purchaser–provider model in the community nursing service.
In each of the municipalities we collected data from a focus group interview with five and four local councillors respectively, each with at least 3 ½ years of experience of sitting on a ‘healthcare committee’. We also collected data from individual interviews with the heads of municipal healthcare services, and from our analysis of municipal documents obtained for the period 2000–2015.
Document searches
The respective municipal documentation systems were accessed through the local authority websites and we searched for political documents that concerned community nursing and home-based care services since the year 2000, using ‘hjemme*’ [“home”] as our search term.
For both municipalities our search produced action plans, financial plans and municipal plans, as well as minutes of meetings: a total of 27 documents in municipality 1 and 29 documents in municipality 2. Our study involved eleven informants and we conducted our interviews between April and July 2015.
Interviews
All interviews were conducted according to the same interview guide. The topics covered by the guide included the organisation of the community nursing service in general, as well as the specific grounds for choosing this organisational model, and the concepts of quality and patient safety in the community nursing service.
During the interview, informants received a written list of six possible factors: ‘research’, ‘earlier experience’, ‘patient safety’, ‘quality’, ‘finance’ and ‘formal recommendations made by the municipal administration’. The factors were discussed in an effort to bring out a range of perspectives.
We recorded all interviews on tape and produced verbatim transcriptions. The data were subjected to an inductive content analysis (13) and the two municipalities were compared. As far as the documents were concerned, this analysis covered only relevant paragraphs from 2015 onwards. Earlier documents gave more of an insight into the history of each municipality in terms of how their community nursing services were organised.
The study was reported to and approved by the Norwegian Centre for Research Data (NSD) (project number 42252).
Results
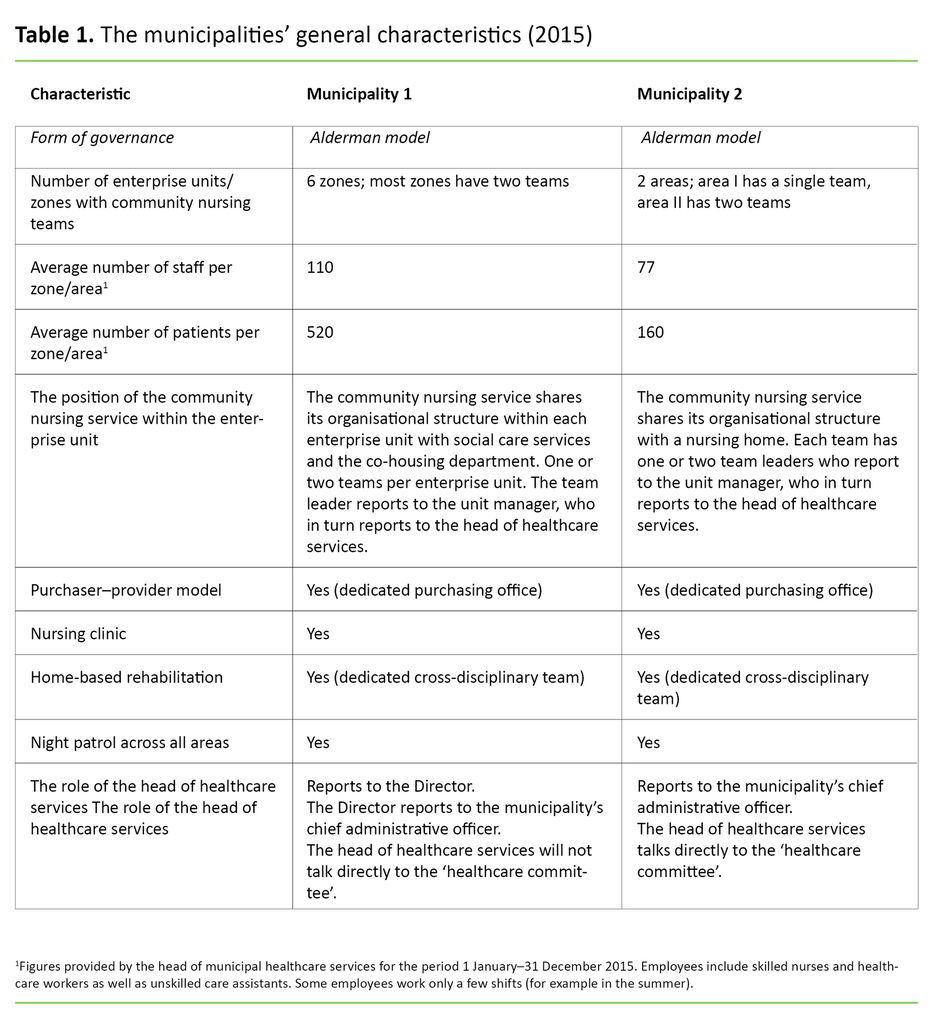
Before we go on to describe the results of the data analysis, table 1 illustrates the characteristics of each municipality.
The reasons given by each municipality for choosing the organisational model of their community nursing service
The documents show that municipality 1 introduced a number of organisational changes in the period 2000–2015. Municipality 1 introduced a ‘profit model’ in 2000, involving a two-tier structure (chief administrative officer and municipal enterprise units) as well as the purchaser–provider model. In 2003, municipality 1 reduced its number of municipal enterprise units from fourteen to eight on ‘discretionary grounds’.
In 2010 the number of municipal enterprise units was reduced from eight to seven, and in 2012 this was further reduced to six in an effort to make each unit more ‘robust’. According to the local councillors in the smallest municipality (2) the team serving area 2 was split for the following reason:
‘It was something they realised was necessary … to enable them to provide a better service …, probably relative to the number of employees, that there were many staff …. And to achieve a better operational structure, they decided to split in two’ (local councillors in municipality 2).
The local councillors in municipality 2 reported that they had not been involved in the decision. Our results show that neither research evidence nor health promotion were factors that impacted on the way that the community nursing service was organised in any of the municipalities, but the formal recommendations made by the administration did have an impact. The local councillors stated that they were completely dependent on these recommendations.
Dominated by financial affairs
The local councillors in municipality 1 said that ‘the plans often looked great’, but that they were required to ‘read between the lines’ because there was insufficient knowledge about whether the plans would work. The local councillors in municipality 1 agreed that financial concerns are at the heart of any reorganisation aimed at saving money. While this factor dominates, the local councillors doubted whether reorganisation does in fact generate savings, since changes are also a drain on resources.
According to the head of healthcare services in municipality 1 the introduction of the purchaser–provider model was an organisational trend, and this individual was uncertain whether the current organisation was founded on concerns for quality or finances. The municipal documents from the period 2003–2015 in this municipality showed that financial concerns were more prominent than concerns for quality.
For example, based on service user surveys conducted in 2005, 2008 and 2010, the municipality concluded that the quality had deteriorated when the purchaser–provider model was introduced due to reduced user involvement, accessibility, reliability and information. Also, patients were required to relate to a greater number of staff.
These user experiences appeared not to have influenced the organisation of the service. The documents gave considerably more prominence to finances than patient experiences, which is why the municipality wished to invest even further in the purchaser–provider model. Our analysis of the data shows that neither earlier experience nor patient safety had been included in the rationale for organisational decision-making in municipality 1, but that in municipality 2 these factors may have had some impact.
Quality was highlighted as an important factor in municipality 2, and all informants from this local authority said that quality had been a prime concern when deciding how the community nursing service should be organised. According to them, this was the reason why one of the teams had been split in two. An overall assessment of findings in both municipalities shows that health promotion (cf. the Norwegian Public Health Act) has had no impact on the current organisation of the community nursing service.
The importance of quality and patient safety
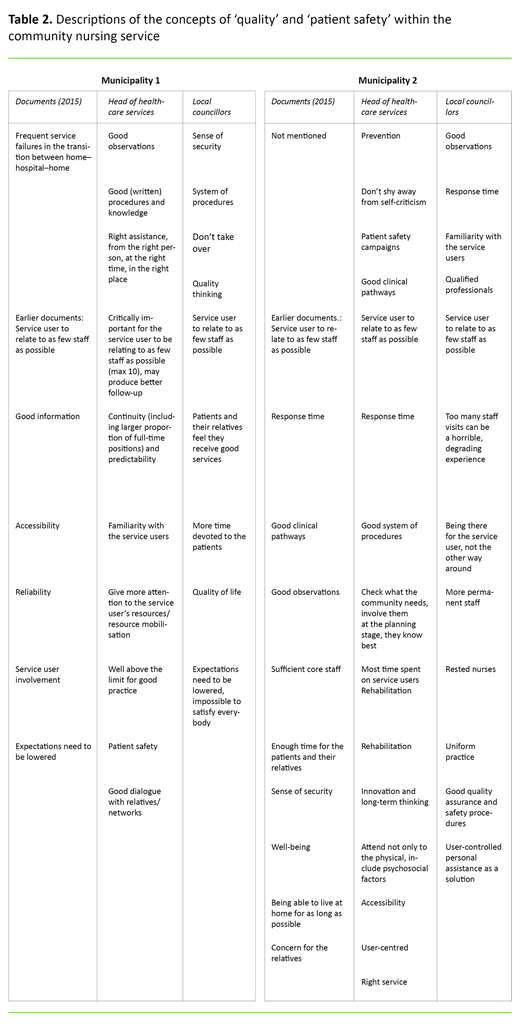
In terms of defining quality and patient safety in the community nursing service, our analysis of the data brings out similarities as well as differences among the informants and in the documents obtained from both municipalities (see table 2).
The head of healthcare services in municipality 2 was the only person who believed that the needs of the population should be mapped with regard to quality improvement initiatives and that the public must be involved with the planning, since ‘they know best’. The informants and documents also mentioned ‘the right help, from the right person, at the right time, in the right place’, qualified professionals, good dialogue with relatives and awareness of psychosocial factors when talking about the nature of quality and patient safety in the community nursing service.
There was agreement across the municipalities that patients should have to relate to as few staff as possible. The local councillors in municipality 1 felt that quality of life was important, and spending more time with patients was key. They argued however that expectations with respect to the standard of service had to be lowered, and that satisfaction among all patients would be impossible. This is reflected in the documents from municipality 1, which show that expectations for an increased standard of services must be lowered due to reduced municipal revenues.
Assessment of how the community nursing service is organised
With respect to the current organisation of the community nursing service, all sources from both municipalities were in agreement that ‘patients currently have to relate to far too many members of staff’. The documents from municipality 1 included multiple references to how team mergers can make the community nursing service more robust and yield financial savings. The head of municipal healthcare services supported this line of thinking:
‘There is a need for the municipality to be subdivided on geographic grounds, but four enterprise units will be more sustainable than six, which will produce a larger pool of employees for making up small teams if that’s desirable’ (head of healthcare services in municipality 1).
Nevertheless, this individual also stated that it is possible to lose control and the overview if the units are too big. The local councillors appeared to be more skeptical towards team mergers out of consideration for staff, who would need to adapt:
‘Then there’s something about the need for constant reorganisation in the health service and other services. As healthcare professionals it’s enough to drive you up the wall… All of these councillors who are constantly thinking of something new in order to make their mark … It’s never-ending. So I’m not saying that we shouldn’t reorganise, but give the professionals a bit of peace and quiet to do their job’ (local councillor in municipality 1).
Different views on the purchaser–provider model
In accordance with the documents, the head of healthcare services in municipality 1 highlighted the purchaser–provider model. The model was described as sensible in light of the requirements for legal protection, but it was made clear that simplification was needed. However, the local councillors in municipality 1 rarely referred to this model and appeared to take a neutral view on it, or they wished to have it abolished for the following reason:
‘The level of bureaucracy is immense [and even] the Norwegian Nurses Organisation considers it to be nonsense … First you need to place an order and then you need to wait for someone else to deliver. Why can’t the same person do both jobs?’ (local councillor in municipality 1)
Among the local councillors it appeared that legal protection and documentation requirements were more important: ‘If you haven’t documented it, just forget it.’
In municipality 2, no mention was made of the purchaser–provider model or of the reporting requirements. All sources were positive to a future merger and co-location of all teams. A merger could not, according to the document, be ‘disadvantageous for the patients’. The head of municipal healthcare services used the word ‘synergy’, but said that the argument against mergers involved a potential that there would be too many members of staff to relate to.
Although the local councillors in this municipality were positive to co-location, multiple teams would provide a better service: ‘… fewer members of staff to relate to.’ The results show that in both municipalities it was only the local councillors who reflected on what the staff felt about the current organisation, and they were concerned about pressures of time and stress, insufficient time spent with patients, dialogue, the exercise of discretion, and excessive financial control.
Discussion
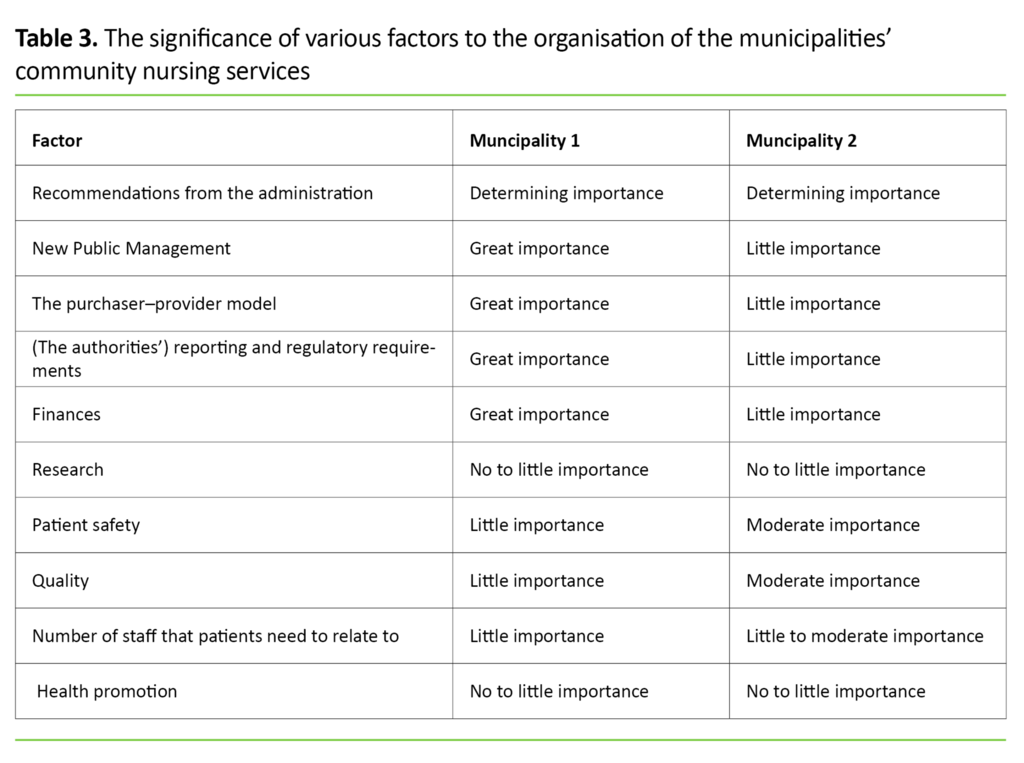
Table 3 provides an overview of all factors and their impact on the municipalities’ organisation of the community nursing service.
Despite the fact that the White Paper about the primary health service of the future (1) expects the organisation of community nursing services to be evidence-based, with a clear emphasis on health promotion (14), our results show that the opposite is the case. The lack of an evidence-based approach may be explained by the fact that research is not an overarching concern when decisions are made (15).
However, the results show that formal recommendations made by the municipal administration are a determining factor in the way that the community nursing service is organised. This may reflect a growing trend ‘that important decisions are transferred away from the local council and over to bodies that are made up of non-elected representatives’, i.e. so-called fragmentation (16, p. 129).
Other studies also describe a development that sees the local council becoming more of a decision-making body (17), with increasingly detailed control being exerted by central government, thereby influencing the decision-making processes considerably (18). The government’s growing reporting requirements are highlighted as an important factor in the decision-making process, but our results showed differences among the informants in this respect.
The head of municipal healthcare services pointed to the purchaser–provider model as an answer to the reporting requirements, while the local councillors queried the model because it led to more bureaucracy; some considered abolishing the model. In a decision-making perspective (3), the results show that different actors have different values and objectives (cf. communicative rationality), while they suggest that the recommendation made by the municipal administration is often the chosen alternative (instrumental rationality) although the local councillors may not necessarily feel that the various options have been sufficiently researched with respect to quality and patient safety.
Criticism of the purchaser–provider model
Earlier research shows that a so-called ‘profit model’ does not bring about better financial control and efficiency, but instead breeds bureaucracy and higher administrative costs (19). An organisation based on New Public Management may lead to higher costs and more complaints (20). Specifically with reference to the community nursing service, the purchaser–provider model has been described in earlier studies as a threat to service user involvement (11) and sound professional practice (21).
Despite this criticism, the head of healthcare services in municipality 1 argued in favour of this model on grounds of legal protection, in line with the documents. This decision may suggest that in municipality 1 the model has benefited from a so-called ‘protective immune resistance’ (22).
In addition to voicing strong criticisms against the purchaser–provider model, earlier research suggests that mergers of community nursing teams may make staff anxious and insecure and may lead to overly complex systems (23). The larger teams formed by team mergers mean that patients will need to relate to a greater number of staff members, and may thereby suffer a risk of experiencing poorer quality and a lower level of patient safety (4).
Studies have shown that autonomous teams consisting of fewer staff may provide a better quality of care and generate a reduced need for care (24), as well as lower costs and more satisfied employees (25, 26). In this light, the findings of our study suggest a number of paradoxes. Several decisions that appear to be rational, do not necessarily have the intended effects (3).
Contradicting arguments in favour of mergers
The arguments in favour of mergers do not coincide with earlier research. In municipality 2, a team was split in two in order to improve quality and reduce the number of staff members that each patient would need to relate to. It is therefore a paradox that this local authority later decided to merge all three teams. The paradox appears to be reinforced by the fact that our sources in both municipalities pointed out that patients already have to relate to too many people.
This paradox may appear to be even greater when we examine the numerical consequences of a team merger. Although table 1 must be interpreted with caution, it is theoretically possible that a patient in municipality 1 is attended to by 110 different members of staff in the course of a single year. Additionally, some patients encounter staff members from the Night Patrol and the rehabilitation service, student nurses and others.
We may ask what this means for the most vulnerable patients whose need for continuity of care is considerable (27). Our study suggests the existence of a management paradox (28) in that the local authorities are more concerned with the continuity of day-to-day operations than with the patients’ need for continuity of care.
Quality and safety at risk
Earlier research suggests that there are different interpretations of the concept of ‘quality’ among front-line staff and decision-makers (29). Our study shows that decision-makers have a broad understanding of what quality and patient safety entail within the context of the community nursing service. They highlight the importance of involving as few members of staff as possible with the care for any single individual (4) as well as the need to employ qualified personnel (6), focus on quality of life (30) and encourage service user involvement (8).
According to the Norwegian government it may seem as if the municipal freedom of choice does not work as intended because the chosen organisational model sometimes fails to meet the legal requirements pertaining to good practice and quality of care (1). In terms of assessing the current organisation of services, the statements made by the local councillors may give the impression that quality and safety are at risk.
We may ask to what extent the legal requirements for sound professional practice can be fulfilled within an organisational structure described as complex and fragmented, where there is a wide gap between decision-makers and patients, and where patients, according to all data sources, are forced to relate to too many staff.
The study has several limitations. Data were collected from only two municipalities, and neither staff nor patients were included in the sample. The first author has been working in the community nursing service since 2003. Both authors contributed to the analysis in order to strengthen its merit and credibility, and to avoid bias.
Conclusion
It was the case in both municipalities that the administration’s formal recommendations had significantly impacted on the way that the community nursing service was organised, while evidence-based knowledge and public health promotion were of limited importance. It seems that the role played by local councillors is marginalised in that they appear on the scene only at the decision-making stage, and the gap between decision-makers and patients is wide.
We identified several differences between the two municipalities. In municipality 1, the purchaser–provider model, reporting and regulatory requirements, and particularly finances, had a significant impact on the way that the community nursing service was organised. These factors were of limited importance in the smaller municipality.
Despite a reasonably broad understanding among decision-makers of the importance of quality and patient safety, these factors were in practice only considered to be of moderate importance in the smaller municipality and of little importance in the larger municipality.
One common denominator was that both municipalities expected the merger of community nursing teams and enterprise units to be beneficial. The fact that they advocated mergers, appears paradoxical since all informants highlighted that patients need to relate to as few members of staff as possible.
In line with more recent White Papers (1, 5), we therefore recommend that municipal decision-makers:
- focus on the quality of services and health promotion in the local community from the citizens’ perspective,
- map the community’s (healthcare) needs, networks and resources, and
- use the two points above as a basis for their organisation and funding of the community nursing service, and the municipality’s organisational structure.
Research suggests that this approach and organisational model may not only improve the health of the local community, but can also generate better satisfaction rates among patients, citizens and staff, in addition to financial savings.
References
1. Meld. St. nr. 26 (2014–2015). Fremtidens primærhelsetjeneste – nærhet og helhet. Oslo: Helse- og omsorgsdepartementet; 2015. Available at: https://www.regjeringen.no/contentassets/d30685b2829b41bf99edf3e3a7e95d97/no/pdfs/stm201420150026000dddpdfs.pdf(downloaded 04.04.2016).
2. Mørk E, Sundby B, Otnes B, Wahlgren M. Pleie- og omsorgstjenesten 2013. Statistikk om tjenester og tjenestemottakere. Oslo, Kongsvinger: Statistisk sentralbyrå; 2014. Available at: http://www.ssb.no/helse/artikler-og-publikasjoner/_attachment/201126?_ts=1499f2338b0(downloaded 20.09.2015).
3. Engen OAH, Kruke BI, Lindøe PH, Olsen KH, Olsen OE, Pettersen KA. Perspektiver på samfunnssikkerhet. Oslo: Cappelen Damm Akademisk; 2016.
4. Institute of Medicine (US) Committee on Quality of Health Care in America. Crossing the quality chasm: a new health system for the 21st century. Washington, D.C.: National Academy Press; 2001.
5. Meld. St. nr. 29 (2012–2013). Morgendagens omsorg Oslo: Helse- og omsorgsdepartementet; 2013. Available at: https://www.regjeringen.no/no/dokumenter/meld-st-29-20122013/id723252/ (downloaded 31.10.2014).
6. Hughes RG, red. Patient safety and quality: An evidence-based handbook for nurses. Rockville, MD: Agency for Healthcare Research and Quality (US); 2008. Available at: https://www.ncbi.nlm.nih.gov/books/NBK2651/(downloaded 30.10.2016).
7. Bredland E, Linge OA, Vik K. Det handler om verdighet og deltakelse: verdigrunnlag og praksis i rehabiliteringsarbeid. 3. ed. Oslo: Gyldendal Akademisk; 2011.
8. Hanssen H, ed. Faglig skjønn og brukermedvirkning i helse- og omsorgstjenestene. 2. ed. Bergen: Fagbokforlaget; 2015.
9. Vabo SI, Stigen IM. Moteslaveri, interesser og behov. En analyse av utbredelsen av «moderne» organisasjonsløsninger i norske kommuner. Nord Organ. 2004;6(1):48–88.
10. Vabø M. Norwegian home care in transition – heading for accountability, off-loading responsibilities. Health Soc Care Community. 2012;20(3):283–91.
11. Vik K, Eide A. Older adults who receive home-based services, on the verge of passivity: the perspective of service providers. Int J Older People Nurs. 2013;8(2):123–30.
12. Yin RK. Case study research: design and methods. 5. ed. Los Angeles: SAGE; 2014.
13. Graneheim UH, Lundman B. Qualitative content analysis in nursing research: concepts, procedures and measures to achieve trustworthiness. Nurse Educ Today. 2004;24(2):105–12.
14. Plochg T, Klazinga NS. Community-based integrated care: myth or must? Int J Qual Health Care. 2002;14(2):91–101.
15. Culyer AJ, Lomas J. Deliberative processes and evidence-informed decision making in healthcare: Do they work and how might we know? Evid Policy J Res Debate Pract. 2006;2(3):357–71.
16. St.meld. nr. 33 (2007–2008). Eit sterkt lokaldemokrati. Oslo: Kommunal- og regionaldepartementet; 2008. Available at: http://www.regjeringen.no/nb/dep/kmd/dok/regpubl/stmeld/2007-2008/stmeld-nr-33-2007-2008-.html?regj_oss=1&id=517539(downloaded 12.12.2014).
17. Ringkjøb H-E, Folkestad B, Offerdal A, Aars J. Demokrati heile vegen – Gode styringsgrep og metodar for folkevalte. Bergen: Stein Rokkand Senter; 2007. Available at: https://www.researchgate.net/publication/242781377_Gode_styringsgrep_og_metodar_for_folkevalte(downloaded 4.12.2018).
18. Baldersheim H, Smith E. Lokalt demokrati uten kommunalt selvstyre?: En publikasjon fra Demokratiprogrammet ved Universitetet i Oslo. Oslo: Abstrakt forlag; 2011.
19. Berge DM. Økonomistyring i resultatkommunen. I: Torsteinsen H, red. Resultatkommunen: reformer og resultater. Oslo: Universitetsforlaget; 2012.
20. Hood C, Dixon R. A government that worked better and cost less?: evaluating three decades of reform and change in UK central government. 1. utg. Oxford: New York, NY: Oxford University Press; 2015.
21. Tønnessen S, Nortvedt P. Hva er faglig forsvarlig hjemmesykepleie? Sykepleien Forskning. 2012;7(3):280–5. Available at: https://sykepleien.no/forskning/2012/10/hva-er-faglig-forsvarlig-hjemmesykepleie(downloaded 14.12.2014).
22. Vabø M. Reformtrender og endringsparadokser. In: Vabø Mia, Vabo SI, ed. Velferdens organisering. Oslo: Universitetsforlaget; 2014.
23. Andersen GR, Westgaard RH. Discrepancies in assessing home care workers’ working conditions in a Norwegian home care service: differing views of stakeholders at three organizational levels. BMC Health Serv Res. 2015;15(1):286. Available at: http://www.biomedcentral.com/1472-6963/15/286(downloaded 21.10.2014).
24. Hussey PS, Schneider EC, Rudin RS, Fox DS, Lai J, Pollack CE. Continuity and the costs of care for chronic disease. JAMA Intern Med. 2014;174(5):742–8.
25. Nandram SS. Organizational innovation by integrating simplification. New York, NY: Springer; 2014.
26. Laloux F. Reinventing organizations: a guide to creating organizations inspired by the next stage of human consciousness. Brussel: Nelson Parker; 2014.
27. Woodward CA, Abelson J, Hutchison B. My home is not my home anymore: Improving continuity of care in homecare. Ontario: Canadian Health Services Research Foundation; 2001.
28. Gjevjon ER, Romøren TI, Kjøs BØ, Hellesø R. Continuity of care in home health-care practice: two management paradoxes. J Nurs Manag. 2013;21(1):182–90.
29. Wiig S, Aase K, von Plessen C, Burnett S, Nunes F, Weggelaar A, et al. Talking about quality: exploring how ‘quality’ is conceptualized in European hospitals and healthcare systems. BMC Health Serv Res. 2014;14(1):478.
30. Nies H. Communities as co-producers in integrated care. Int J Integr Care. 2014;14(2):1–4.










Comments