Mapping of procedures for set-up of instruments in the sterile field for surgery
National and multi-regional hospitals appear to use procedures for set-up of instruments in the sterile field more often than local and regional hospitals.
Background: During a surgical intervention, the patient and the surgical team are placed in a situation of calculated risk. Safe teamwork, work processes that follow quality-assured procedures and use of safety equipment may reduce the incidence of complications and injuries.
Objective: The objective of the study was to help achieve best practice and avoid adverse events associated with the set-up and organisation of instruments in the sterile field. We therefore identified the current status in Norwegian surgical departments and investigated correlations with the functional level of the hospital.
Method: We used an online survey. The mapping study was undertaken in 16 hospitals and included all health regions and hospitals at all functional levels.
Results: All the surgical departments used procedure cards, tray lists, counting procedures and procedures for dealing with sharps injury. Written procedures describing set-up of the instruments in the sterile field were used in four hospitals. Hospitals that provide national or multi-regional services rely on procedures to the greatest extent.
Conclusion: The results point to a correlation between the hospitals’ service profile and deficiencies when it comes to procedures for the set-up of instruments in the sterile field. We recommend that evidence-based guidelines and procedures be established. Furthermore, we recommend that the evidence base for set-up of instruments in the sterile field be examined.
It has been estimated that in 2012, a total of 312.9 million surgical procedures were undertaken worldwide (1). Studies from industrialised countries show that serious complications occurred in 3–22 per cent of all surgical procedures (2). In a surgical team, the operating room nurses are assigned key tasks that involve control, overview and clinically correct handling of instruments and equipment, all of which are crucial for the safety of the patient and the personnel.
The ‘Safe Surgery’ checklist has helped reduce the number of complications associated with surgical interventions (3) and ensure that procedures are defined and complied with. The checklist confirms that the instruments are sterile and available, and that the number of instruments and other pieces of equipment tallies before and after the intervention (2). This control is reliant on quality-assured, updated and applied evidence-based procedures.
The requirement for an evidence-based approach is intended to help provide practitioners with the best possible basis for decision-making (4). The study by Hjelen and Sagbakken (5) pointed out that an organisational structure and culture that undermines evidence-based practice (EBP) exists in Norwegian surgical departments and training institutions.
The authors of the study undertook focus-group interviews showing that the theatre nurses lacked competence in EBP. They are facing time constraints that cause them to give low priority to such work. In addition, they call for facilitation and time to devote to competence enhancement and want to make use of evidence-based knowledge (5).
Guidelines for set-up of instruments in the sterile field
Guidelines related to the organisation and set-up of instruments and equipment are prepared by large national professional organisations for operating room nurses and technicians, such as the Association of periOperative Registered Nurses (AORN) (6) and the Association of Surgical Technologists (AST) (7).
In Europe and the USA, methodological quality assurance of guidelines is mainly undertaken by the Guidelines International Network (GIN) in Scotland, the National Institute for Health and Care Excellence (NICE) in the UK and previously by the National Guideline Clearinghouse (NGC) in the USA. Professional organisations and regulatory agencies jointly help establish and promote the use of evidence-based recommendations (8).
In Norway, the Directorate of Health has a mandate to prepare national guidelines that describe good clinical practice and how regulations are to be interpreted. The Directorate of Health wishes for more coordination between service locations and levels, and has prepared a manual to ensure transparent processes for the development of evidence-based guidelines (9). No Norwegian guidelines have been prepared to regulate the perioperative planning and facilitation of how to set up instruments in the sterile field in the context of surgical interventions.
Development and approval of clinical procedures
Clinical procedures are developed and approved by the health trusts and can be sent to the Norwegian Electronic Health Library’s website for clinical procedures (10). Quality assurance by the Norwegian Electronic Health Library ensures that recognised methods have been used in the preparation of clinical procedures, and that the procedures that meet the requirements are published (11).
In 2009, the Norwegian Knowledge Centre for the Health Services identified approximately 46 000 clinical procedures in Norwegian health trusts. The procedures were methodologically weak, both internally and externally uncoordinated, and inadequately updated (12). A follow-up study undertaken in 2016 showed that the number had risen to approximately 99 000 procedures. The study showed that there was uncertainty regarding the quality of these procedures, a large proportion of them were not updated, and there was uncertainty regarding the extent and nature of their use (13).
In operating room nursing, oral communication and collegiate supervision have a long tradition and may help develop experience-based knowledge, which is a key component of EBP. In principle, such an oral routine is nevertheless insufficient. Students find that supervisors differ in their descriptions of ways to set up the instruments in the sterile field. The students therefore call for a standardised set-up (14).
Objective of the study
There is a need for an evidence-based, consistent and rigorous regimen around the preparation for surgery, a rational set-up of the instruments in the sterile field and safe collaboration within the surgical team. The objective of this study was to help achieve best practice and avoid adverse events associated with the set-up and organisation of the instruments and equipment for surgical interventions.
The study’s target group includes those who are responsible for setting up and handling instruments in the sterile field and those who develop procedures for this. The study also addresses hospital managers with responsibility for quality assurance. At the national level, the study is aimed at professional organisations, health trusts and agencies responsible for developing evidence-based guidelines.
Moreover, we wanted to describe the procedures that are applied in connection with the set‑up and organisation of instruments in the sterile field in Norwegian surgical departments, and how the procedures are distributed among the different service levels of the hospitals.
We investigated the following research question:
What procedures do surgical departments in Norwegian hospitals apply in connection with the set-up and organisation of instruments in the sterile field, and how are these procedures distributed among hospitals?
Definition of the hospitals’ service profiles
Norway is divided into four health regions/authorities: Northern Norway Regional Health Authority, Central Norway Regional Health Authority, Western Norway Regional Health Authority and South-Eastern Norway Regional Health Authority (15). The health authorities distribute service provision between the hospitals and presuppose close collaboration to cover needs in the catchment area. The four regional hospitals – University Hospital of North Norway, St. Olavs Hospital Trondheim University Hospital, Haukeland University Hospital and Oslo University Hospital – have the broadest range of services in the health regions (16).
Norwegian hospitals provide different kinds of services to the patients, and thus have varying functional levels. The top level comprises national and multi-regional treatment services and national advisory services. ‘The examination and treatment of a small group of patients that require highly specialised competence or use of specialised medical equipment’ are centralised to one or two locations in the country (17, p. 4). The Ministry of Health and Care Services is charged with approval and implementation of national services, cf. the manual National Services in the Specialist Healthcare Service (17).
The National Health and Hospital Plan uses the designations ‘large emergency hospital’, ‘emergency hospital’ and ‘hospital without emergency functions’. A large emergency hospital has a catchment area of more than 60–80 000 inhabitants and a broad range of emergency services, including emergency surgery and numerous medical specialties.
Emergency hospitals have a minimum emergency function for internal medicine, an anaesthesiologist on 24-hour duty, planned surgery and also emergency surgery if factors such as geography, distance to the hospital, required services such as vehicle, boat or air transport or weather conditions make this necessary. Hospitals without emergency functions undertake planned treatment that does not require such functions (16).
Designations for recommendations
The objective of clinical recommendations in the health services is to provide quality assurance and standardise the activities, and according to Nylenna (18), the designations for such recommendations should be subject to better quality assurance and standardisation. Designations for the specific recommendations that are used in the hospitals’ methodology books include ‘manual’, ‘guideline’ and ‘procedure’ (18).
A manual is a general document that provides guidance in a broad range of areas (organisational and medical) and sets out general recommendations for a large target group. Manuals can also provide elaborations on regulations and descriptions of recommended forms of organisation (18). A guideline, on the other hand, tends to have a more narrowly defined and action-oriented content. Guidelines will often be prepared systematically and include normative recommendations for dealing with clinical issues or situations (18).
A key concept in this study is ‘procedures’, which can be of a medical or administrative nature. According to Nylenna (18) they are more delimited and detailed than guidelines, and are defined by Standards Norway as ‘a course of action to perform an activity or a process’ (18, p. 2). Procedures describe specifically how delimited tasks ought to be performed, and may also state who should perform the task in question and where equipment can be found (18).
In this article, ‘procedures’ is used as a collective term for all documents that in various ways can describe or provide guidance for activities that are included in the handling of equipment in the sterile field. In this article we do not distinguish between ‘procedures’ and ‘clinical procedures’ as used on the Norwegian Electronic Health Library’s website.
Method
The study design is an exploratory cross-sectional survey (19) that examines the state of the procedures applied in the sterile field in surgical departments in Norwegian hospitals at the time of the survey from November to December 2017. The exploratory design meant that some hospitals and departments were selected. We used an online survey to collect the data.
Sample
An overview of the country’s four health regions with health trusts and hospitals was retrieved from the government website regjeringen.no under the topic ‘Hospitals’ (15). The target group consisted of hospitals, and the choice of hospitals was strategic (19). The included hospitals should represent health trusts from all the four health regions and all levels of service provision in order to prevent culture from having an influence on the study, including in the sense of system-related influence from the hospitals and the impact of educational institutions on health trusts and hospitals.
In this study, hospitals designated as ‘large emergency hospitals’ are categorised as hospitals with a regional function, and hospitals without emergency functions and emergency hospitals with or without an emergency surgery department are categorised as local hospitals. The categorisation was related to information on the health trusts’ websites and the alternatives chosen by the participants.
One hospital was contacted by telephone to obtain information on its service profile. The Ministry of Health and Care Services provided an overview of health trusts and hospitals with national and multi-regional service coverage (17). In light of the Ministry’s manual, two hospitals were re-categorised as providers of national and multi-regional services.
If more than one service level had been selected in the questionnaire, the hospital was categorised at the highest level indicated. We ensured a representative sample (19) consisting of five local hospitals, seven hospitals with a regional function and four hospitals with national or multi-regional treatment services (previously national functions). Moreover, all health regions were included.
We contacted the hospitals by telephone, and contact was established with relevant heads of surgical departments. Depending on the organisational structure in each hospital, the heads of division or department granted permission and responded to the survey or gave the name of a contact person who assisted in the survey process.
Sixteen out of 18 hospitals (89 per cent) responded to the survey after a total of two reminders. In general, the risk of bias will be minor in a survey that uses regular mail and has a response rate of more than 65 per cent (19), and we can assume that this also applies to online surveys.
The two hospitals that did not respond included one hospital with national and multi-regional services and one hospital with regional functions. Those who did not respond are not considered to be different from those that participated. We thus assume that this has caused no bias in the results (19).
The instrument – online survey
Few resources are available for developing a customised instrument, and Polit and Beck recommend using previous surveys that are relevant for the survey in question (19). The authors were unable to find a suitable instrument and therefore prepared an online survey with guidance from the IT personnel at the University of Tromsø. Questions and response categories were developed by the first and third authors in collaboration. Both have long-standing experience and familiarity with the area of operating room nursing and associated clinical practices.
The instrument was pre-tested by four operating room nurses from two Norwegian health regions. The pilot project showed a good correspondence between the way in which the questions were interpreted and the issues that the study wished to examine.
The survey was designed as a structured self-reporting instrument with structured, closed-end questions and pre-defined response alternatives (19). See Table 1 for further details. The participants could choose multiple categories (alternatives) for each question.
The mapping was undertaken with the aid of a tool for the design and implementation of online surveys called Nettskjema. This solution is developed and operated by the University Center for Information Technology (USIT) at the University of Oslo (20). The title of the survey undertaken in this study was ‘Organisation/set-up of instruments and equipment on the Mayo stand and back table for surgical interventions’.
Ethical considerations
Since the questions in the mapping are regulated by the Freedom of Information Act and did not involve the processing of personal or health information, the project was not subject to the duty to notify the Norwegian Centre for Research Data (NSD) or the Regional Committees for Medical and Health Research Ethics (REK). The project was presented by telephone to a contact person or head of the surgical department or division to provide an opportunity to clarify any issues involved.
Written information was submitted along with a request for participation and a link to the survey. The Nettskjema solution is designed to fulfil all Norwegian requirements for data protection (20). Participation was voluntary, and a completed response was considered to constitute consent. Names of hospitals were treated confidentially and anonymised.
Analysis
We analysed the results with the aid of descriptive statistics (19). The target group for the study was hospitals, and the available study population consisted of surgical departments. Procedures (the variable) were operationalised in mutually exclusive categories (19) and included the category ‘Other’ to ensure that the list was exhaustive.
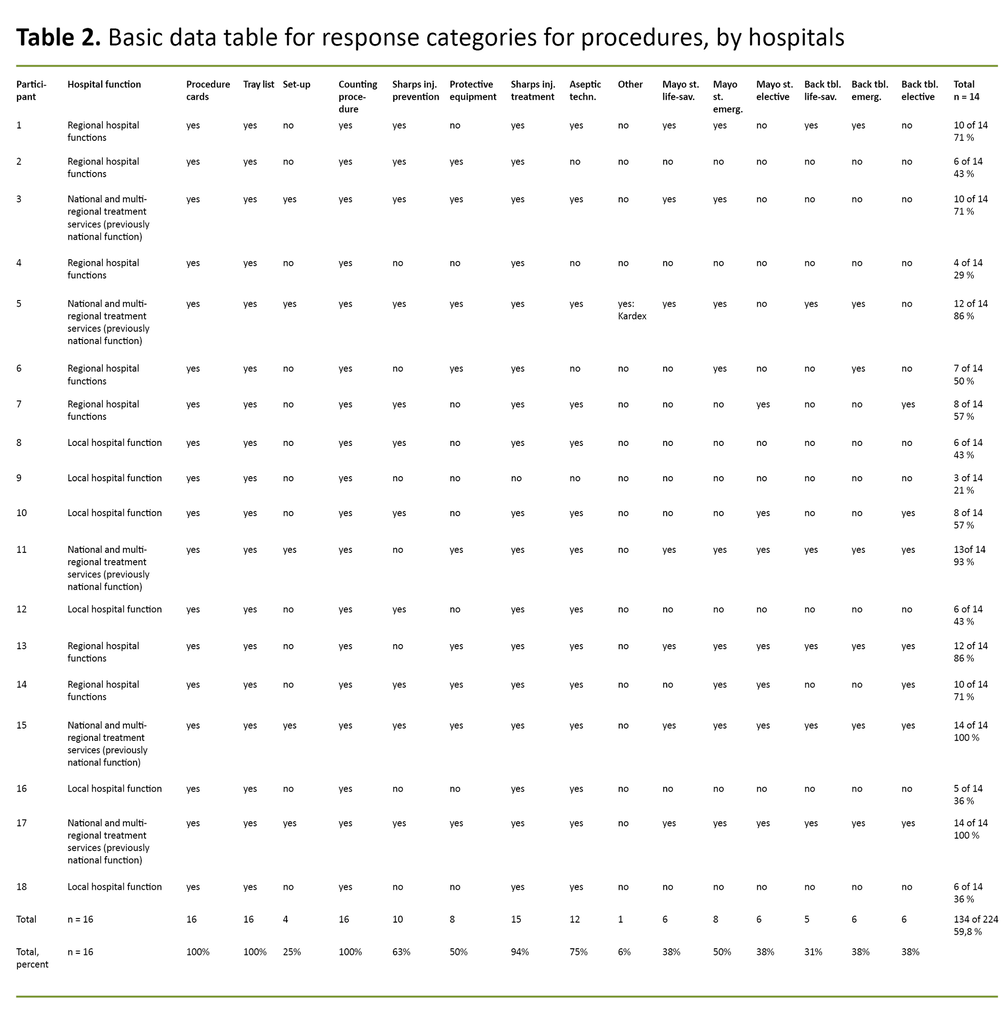
Only one hospital selected the alternative ‘Other’. The authors decided that the described alternative overlapped with the category ‘Procedure cards’ (Table 2).
The results from the survey were available in Nettskjema and calculated as percentages. In addition, the responses were analysed in Excel with the aid of pivot tables. Categories (response alternatives) were coded into abbreviations that were used for data processing and tabular presentations, see the alternatives in Table 1 and response categories in Table 2. The responses were converted into a numerical format through a stepwise coding: the selected alternative was coded as ‘yes’ and further as ‘1’, whereas the alternatives that had not been selected were coded as ‘no’ and further as ‘0’.
On the basis of this coding, we prepared an initial table that showed how the procedures were distributed among the individual hospitals; see Table 2 for further details. The initial table was then transferred to pivot tables, in which we combined the hospital’s function with the chosen categories for procedures and images.
Results
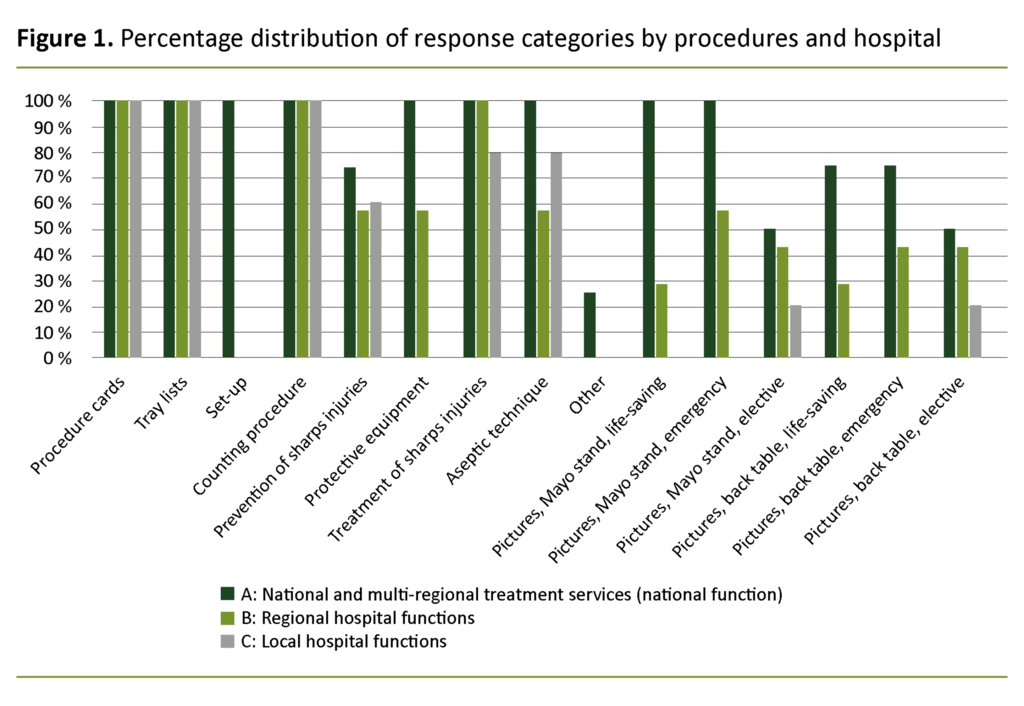
The results show what procedures are applied and how these are distributed among the hospitals (Table 2), as well as the percentage distribution of procedures by the functional level of the hospital (Figure 1). The results show that local hospitals and hospitals with regional functions use procedures less frequently. The study indicates that high-level hospitals with national and multi-regional treatment services rely on procedures to a greater extent than hospitals at a lower functional level.
On average, hospitals with national and multi-regional treatment services apply 75 per cent of the procedures in this study. Hospitals with regional functions apply on average 58 per cent and local hospitals on average 40 per cent of the procedures, according to a calculation of percentages based on Table 2.
The mapping study also identifies procedures that the participants in this study indicate that they use, irrespective of hospital function. All hospitals, with the exception of one local hospital, apply the following procedures: procedure cards, tray lists, counting procedures and procedures for dealing with puncture wounds, see Table 2 and Figure 1.
The results show that local hospitals do not apply the procedure for protective equipment, and that the procedure for the prevention of puncture wounds is applied least often in hospitals with regional functions. This procedure was also the only written procedure that not all hospitals with national and multi-regional treatment services applied (Table 2).
Furthermore, the results show that 100 per cent of the hospitals with national and multi-regional treatment services and 80 per cent of the local hospitals apply a procedure for aseptic technique. Surprisingly, the results show that only 57 per cent of the hospitals with regional functions apply a procedure for aseptic technique (Figure 1).
Procedures for set-up of instrument trays
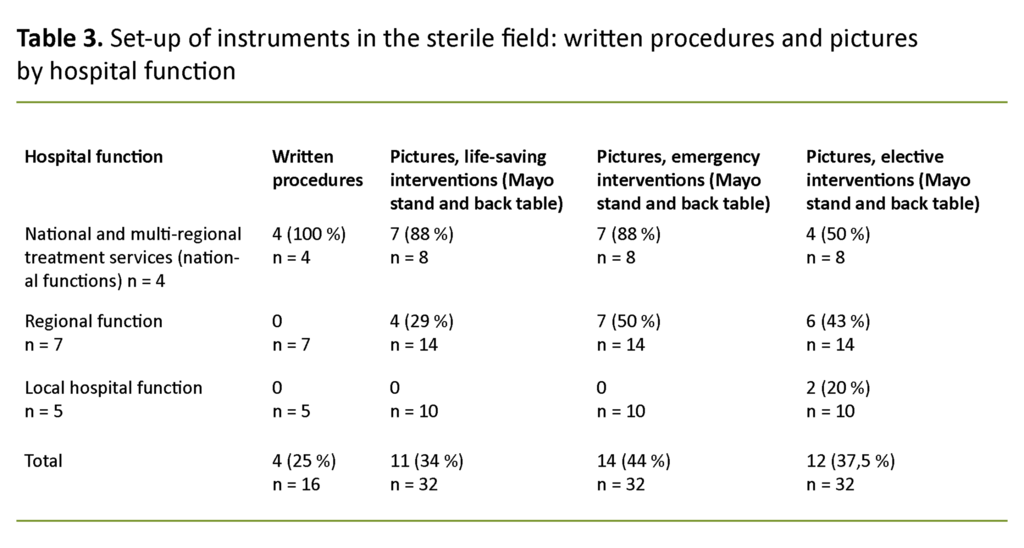
Written procedures and pictures are used to describe the recommended set-up of instruments in the sterile field for different surgical interventions. These procedures have the lowest total scores in this study and showed the greatest differences between hospitals with different service profiles (Table 3).
Table 3 shows that hospitals with national and multi-regional treatment services are the only ones to apply written procedures for set-up of instruments in the sterile field. Moreover, Table 3 shows that these hospitals also use pictures to demonstrate set-up of instruments in the sterile field more frequently than the others, and that the use of pictures declines in pace with the level of the hospital’s service profile. Only one local hospital included in this study uses pictures.
The trend for the two upper hospital levels shows only a minor difference between pictures of the Mayo stand versus back table, or when it comes to categories for life-saving help, emergency help and elective surgery. See Table 3 for details.
Discussion
Good quality in the services to patients is essential, and updated and adequate use of knowledge is a precondition. Teaching in educational institutions and practical supervision in clinical settings are required to rely on evidence-based practice (21).
Practical supervision relies on evidence-based procedures and assumes that all health trusts have prepared quality-assured procedures. According to the manual from the Directorate of Health, evidence-based guidelines help healthcare workers and patients make decisions, reduce unwanted variation and promote high quality (9).
There is consensus that appropriate implementation of the ‘Safe Surgery’ checklist contributes to better patient outcomes (3). One key objective of the checklist is to ensure that necessary procedures have been followed (2). This presupposes that quality-assured procedures exist and are correctly applied.
This study showed that the participating hospitals have prepared and apply numerous procedures that are important in the context of surgical interventions. On the other hand, the study shows that only four of the participating hospitals applied written procedures that include recommendations for set-up of instruments in the sterile field for various surgical operations. All of these four hospitals provided national and multi-regional services (national functions).
The same four hospitals also used pictures of instrument trays when preparing for various surgical operations to the greatest extent. The study indicates that there is a difference in functional level between hospitals with different service profiles when it comes to how procedures are applied in setting up and organising instruments in the sterile field.
This continues to happen despite the fact that students point out that instruments in the sterile field are set up differently by different supervisors, and despite their call to standardise the setting up of instruments in the sterile field for different types of surgical interventions (14).
Ensure that necessary and quality-assured procedures are developed
Our experience from searches for guidelines and standards shows that a variety of search terms need to be used in the various databases, and this makes literature searches a time-consuming affair. Unavailable and costly full-text articles exacerbate this problem and complicate the preparation of evidence-based procedures. Operating room nurses feel that they lack competence in searching for literature and selecting databases, they have difficulty reading research material in English, and request more time to devote to this work (5).
Networks for evidence-based procedures provide a recognised method for preparing procedures and offer assistance in this process (11), and they also make the procedure generally available on the knowledge centre’s website (10). Competence development and a sharing culture can help ensure that health trusts do not need to develop the same procedures, and can enable quality assurance of the procedures. Training, time and opportunities for competence development are needed to fulfil the requirements for developing evidence-based procedures, including literature searches and use of the methodology assessment tool AGREE II (11).
Good projects are welcome. The University Hospital of North Norway implemented a training programme for nurses and managers in which they were introduced to evidence-based practice and learned about preparing procedures. As a result of these training sessions, procedures were revised and are now evidence-based (22). Similarly, the launch of master’s degree programmes in operating room nursing may help increase the students’ competence in applying evidence-based knowledge.
The web pages of the Norwegian Electronic Health Library show no trace of a sharing culture when it comes to procedures for work in the sterile field. No evidence-based guidelines for setting up instruments are available, and only a single evidence-based procedure is available, applicable to surgical counting (23). Each health trust is nevertheless responsible for developing evidence-based procedures.
The results from this study show the procedures that are applied. We point to shortcomings and indicate that there are differences between the hospitals in terms of their functional levels when it comes to application of procedures. The study did not investigate the quality of these procedures. On the other hand, it is worth noting the alarming results in terms of the huge volume of procedures that have been prepared, as well as the poor quality and insufficient coordination of procedures in Norwegian health trusts (12, 13). It is reasonable to assume that these results are also representative for the surgical departments, and this assertion is supported by the operating room nurses’ explicit need for competence in EBP (5).
Based on this study, the authors recommend that evidence-based guidelines be prepared, as well as procedures that can help provide quality assurance and reduce variations when it comes to set-up and organisation of instruments in the sterile field in Norwegian surgical departments.
The regional hospitals, which provide the broadest range of services and have the best competence, are encouraged to collaborate in preparing evidence-based guidelines and procedures and making them generally available on the web pages of the Norwegian Electronic Health Library. Similarly, we challenge hospital managers and heads of surgical departments to ensure quality assurance of the work on procedures by providing operating room nurses with thorough training and opportunities for developing competence in EBP, as well as practical facilitation and time to prepare evidence-based procedures.
Methodology discussion
The responses that were given are assumed to be representative for the surgical activities of the hospitals. On the other hand, the study is based on self-reporting, with the methodological caveats that are associated with this approach (19).
The reliability of the study may have been affected by the management level that participated. Moreover, the selection of departments and surgical specialties may have had an impact on the results. One weakness of the study is that we did not investigate what kinds of specialties are included in the responses. Future studies should examine selected surgical specialties, and procedures should be examined for variations in scope and content. We also recommend that validated measurement instruments be developed.
Conclusion
The results of this study do not provide a basis for speaking on behalf of all surgical departments in all Norwegian hospitals. The results nevertheless provide good indications that the results should be followed up by further studies. We recommend that future studies be undertaken in a larger sample of hospitals and departments to enable examination of variations at the national level and between surgical specialist departments.
The study revealed that 12 out of 16 surgical departments that participated in the study did not apply written procedures for set-up of instruments in the sterile field. All of the four hospitals that did apply such procedures were providers of national and multi-regional treatment services. The study indicates differences between hospitals in terms of the functional level of their service profiles.
Ultimately, the results of the study concern the safety of patients who are in an extremely vulnerable situation. Access to evidence-based guidelines and standardised procedures and techniques help prevent human error (24).
The operating room nurses’ basis for decision-making can be strengthened by developing evidence-based guidelines and procedures for set-up and organisation of instruments in the sterile field. This may help increase patient safety when surgical interventions are undertaken.
We would like to express our sincere gratitude to all surgical departments that participated in the study.
References
1. Weiser TG, Hayes AB, Molina G, Lipsitz SR, Esquivel MM, Uribe-Leitz T, et al. Size and distribution of the global volume of surgery in 2012. Bull World Health Organ. 2016;94(3):201–9.
2. World's Health Organization. WHO guidelines for safe surgery 2009: safe surgery saves lives. Geneva: World's Health Organization; 2009. Available at: http://apps.who.int/iris/bitstream/10665/44185/1/9789241598552_eng.pdf(downloaded 11.11.2017).
3. Haugen AS, Wæhle HV, Almeland SK, Harthug S, Sevdalis N, Eide GE, et al. Causal analysis of World Health Organization's Surgical Safety Checklist implementation quality and impact on care processes and patient outcomes: secondary analysis from a large stepped wedge cluster randomized controlled trial in Norway. Ann Surg. 2019;269(2):283–90.
4. Nortvedt MW, Jamtvedt G, Graverholt B, Nordheim LV, Reinar LM. Jobb kunnskapsbasert! En arbeidsbok. 2. ed. Oslo: Akribe; 2012.
5. Hjelen W, Sagbakken M. Operasjonssykepleiere mangler tid og kompetanse til å arbeide kunnskapsbasert. Sykepleien Forskning. 2018;13(69422)(e-69422). DOI: 10.4220/Sykepleienf.2018.69422
6. Association of periOperative Registered Nurses, AORN. About AORN. Available at: https://www.aorn.org/Aorn-org/about-aorn(downloaded 08.03.2018).
7. Association of Surgical Technologists, AST. Available at: https://www.ast.org/AboutUs/About_AST/(downloaded 08.03.2018).
8. Clayton JL, Miller KJ. Professional and regulatory infection control guidelines: collaboration to promote patient safety. AORN Journal. 2017;106(3):201–10.
9. Veileder for utvikling av kunnskapsbaserte retningslinjer. IS-1870. Oslo: Helsedirektoratet, 2012. Available at: https://helsedirektoratet.no/retningslinjer/veileder-for-utvikling-av-kunnskapsbaserte-retningslinjer(downloaded 08.05.2018).
10. Fagprosedyrer. Oslo: Helsebiblioteket. Available at: https://www.helsebiblioteket.no/fagprosedyrer(downloaded 08.05.2018).
11. Metode og minstekrav for utarbeidelse av kunnskapsbaserte fagprosedyrer. Fagprosedyrer. Oslo: Helsebiblioteket; 17.10.2018. Available at: https://www.helsebiblioteket.no/fagprosedyrer/lage-og-oppdatere-fagprosedyrer/metode(downloaded 08.05.2018).
12. Eiring Ø, Pedersen MS, Borgen K, Jamtvedt G. Prosedyrearbeid – meningsløst mangfold? Notat fra Kunnskapssenteret. Oslo: Nasjonalt kunnskapssenter for helsetjenesten; 2010.
13. Strand G. Prosedyrearbeid – fortsatt meningsløst mangfold? Om arbeid med fagprosedyrer i helseforetak i Norge. (Masteroppgave.) Oslo: Universitetet i Oslo, Det medisinske fakultet, Institutt for helse og samfunn; 2016. Available at: https://www.duo.uio.no/handle/10852/54050 (downloaded 08.05.2018).
14. Igesund U. Studenters deltakelse i kunnskapsbasert fagutvikling: pilotprosjekt i steril-assistanse ved videreutdanning i operasjonssykepleie. Nor tidsskr helseforsk. 2016;12(1):115–28.
15. Regjeringen. Oversikt over landets helseforetak. Oslo; 2016. Available at: https://www.regjeringen.no/no/tema/helse-og-omsorg/sykehus/innsikt/oversikt-over-landets-helseforetak/id485362/(downloaded 08.03.2018).
16. Meld. St. nr. 11 (2015–2016). Nasjonal helse- og sykehusplan (2016–2019). Oslo: Helse- og omsorgsdepartementet; 2015.
17. Nasjonale tjenester i spesialisthelsetjenesten: Veileder. Oslo: Helse- og omsorgsdepartementet; 2017. Available at: https://www.regjeringen.no/contentassets/3b2da09c60e9471c9975fe566416017d/20170131_veileder_nasjonale_tjenester.pdf(downloaded 08.03.2018).
18. Nylenna M. Veileder, retningslinje, prosedyre. Tidsskr Nor Legeforen. 2018;138(2):178–9.
19. Polit DF, Beck CT. Nursing research: generating and assessing evidence for nursing practice. 10. ed. Philadelphia: Wolters Kluwer; 2017.
20. Universitetets senter for informasjonsteknologi (USIT) ved Universitetet i Oslo. Hva er Nettskjema? Oslo; 08.06.2010. Available at: https://www.uio.no/tjenester/it/applikasjoner/nettskjema/mer-om/(downloaded 22.01.2018).
21. Meld. St. nr. 16 (2011–2015). Nasjonal helse- og omsorgsplan. Oslo: Helse- og omsorgsdepartementet; 2011.
22. Liland H-I, Moe V, Thomassen S, Lind R. Jobber og underviser kunnskapsbasert. Sykepleien. 2017;105(8):44–7. DOI: 10.4220/Sykepleiens.2017.63441
23. Kirurgisk telling. Fagprosedyrer. Oslo: Helsebiblioteket. Available at: https://www.helsebiblioteket.no/fagprosedyrer/ferdige/kiriurgisk-telling-anbefalte-rutiner-for-telling-av-utstyr-under-kirurgi(downloaded 02.11.2018).
24. Wahr JA. Operating room hazards and approaches to improve patient safety. UpToDate; 26.03.2019. Available at: https://www.uptodate.com/ (downloaded 23.08.2019).











Comments