Cystic fibrosis: parents’ experiences of informing their children about the disease
Summary
Background: Healthcare personnel who treat parents with a serious health condition, such as cystic fibrosis (CF), must help ensure that the children receive information about the disease. However, the specialist health service provides few good procedures for giving structured information to under-age relatives.
Objective: To obtain knowledge about parents with cystic fibrosis (CF) and their experiences of informing their children about the disease, as well as their expectations of healthcare personnel in this context.
Method: The study has a qualitative descriptive design. Semi-structured interviews were conducted with sixteen cystic fibrosis patients. We carried out a thematic content analysis of the data material.
Results: Patients with cystic fibrosis are selective in terms of who they tell about their disease. Young children received information through two-way communication in casual conversations between child and parent. The parents were unprepared for the children’s existential questions, and older children and teenagers had little knowledge about cystic fibrosis. The parents did not expect healthcare personnel to be able to assist them in providing their children with simple information. The study found that the informants needed more knowledge about their own disease so they can better inform their children.
Conclusion: There is a need for parents to receive structured training in cystic fibrosis. The children must be taught about their parents’ disease, and the information provided must be adjusted to the child’s age and level of maturity. The specialist health service must be more alert to their responsibility to ensure that children receive information about their parents’ disease.
Cite the article
Homme J, Bakkeheim E, Finstad P, Leegaard M. Cystic fibrosis: parents’ experiences of informing their children about the disease. Sykepleien Forskning. 2023;18(92358):e-92358. DOI: 10.4220/Sykepleienf.2023.92358en
Introduction
Cystic fibrosis (CF) is an autosomal recessive inherited progressive disorder (1) that can affect multiple organs, such as the pancreas, bowels, liver, and lungs. Some patients have mild symptoms, while others become seriously ill (2). Pulmonary disease is the main cause of premature death and accounts for 95 per cent of the mortality (3).
In recent decades, improved diagnostics and treatments have considerably extended the life expectancy of CF patients (4). They now have an opportunity to go to school and to have a working life. Many have higher education, work part time or full time and have their own family, although they live with the threat of developing serious disease (4, 5).
Pulmonary physiotherapy is a key part of preventive CF treatment programmes. Most people with CF are treated with pancreatic enzymes to improve their uptake of nutrients. Those who recognise known complications, such as infections and reduced pulmonary function, at an early stage, will have better treatment outcomes. Outpatient consultations, hospitalisation and lengthy home-based treatments impact on the patients’ daily routines and their quality of life (1, 4).
Many people with CF wish to become parents. The parenting role is affected by the chronic disease, which lays claim to much time and personal effort. Those who want children should plan this in consultation with the treating doctor (6, 7). The couple must be informed about CF inheritance and the healthy partner must be offered genetic analysis. The child will be a genetic carrier of the disease, which may affect them later in life.
Healthcare personnel have a duty to help provide information to children whose parents or siblings are patients with a mental health disorder, substance dependence, serious somatic illness or injury (8). Multiple earlier studies have focused on children with CF, how parents deal with having a child with CF (2, 9, 10), and how parents with CF need to balance their time between caring for their child and caring for themselves (7).
We are not aware of any existing research on how parents with CF inform their children about the disease. Research on parents living with cancer and multiple sclerosis (MS) is of relevance, since these are also serious illnesses with an uncertain prognosis. As is the case with CF, cancer treatment and MS exacerbation can lead to hospitalisation, leaving the child separated from the people caring for them (11, 12).
Cancer in parents can cause psychosocial stress in children and a fear of losing the person who is ill (11). Emotional problems in parents with MS increase the risk of their children developing mental health problems (13). Communication about the parents’ disease is a process that should start at an early age and continue through the children’s stages of development.
Objective of the study
We wanted to obtain knowledge about parents with CF and their experiences of informing their children about the disease, as well as their expectations of healthcare personnel in this context.
Method
Study design
The study has a qualitative descriptive design (14, 15). Semi-structured interviews (16) were conducted, and the material gathered was subjected to a qualitative content analysis (15). The study design involves comprehensive syntheses of phenomena, referred to as situations in colloquial language (14). Qualitative content analysis was chosen because the findings can be described as a synthesis of the informants’ experiences (16). The study was a quality improvement project, and the purpose of the analysis was primarily to describe rather than investigate data in an interpretive manner (15).
Sample
The patients were recruited when attending Oslo University Hospital for medical check-ups. The inclusion criterion was confirmed CF diagnosis before having had biological or adopted children. We included 16 adults: twelve women aged between 29 and 63, and four men in the 42–54 age range. Combined, they had 30 children aged between twelve months and 30 years (27 biological and three adopted). The parent with CF was interviewed. Patients were included irrespective of the severity of their illness. Their marital status was not recorded.
We prepared an interview guide consisting of the following questions:
- How do you feel about telling other people about your condition?
- What have you told your children about having CF?
- What age was the child when the information was first provided?
- What are your expectations of healthcare personnel in terms of providing your children with information about your disease?
Conducting the interviews
An experienced specialist CF nurse conducted the interviews in the period between December 2014 and May 2015 at Oslo University Hospital’s pulmonary outpatient clinic. Audio recordings were made of all conversations, one interview per participant. We used an interview guide where we focused on the information provided to children by their own parents. We put an emphasis on openness in all our conversations, to encourage patients to talk about their own experiences. Interview duration was between 30 and 60 minutes.
Qualitative content analysis
The analytic process started during the interview (17). All interviews were transcribed verbatim. This was followed by spot checks, which involved us reading excerpts of the transcript while playing the audio recording (18, 19). We identified meaning units within the text, based on the study’s research questions. These units were verbatim quotes and represented the transcript’s manifest content.
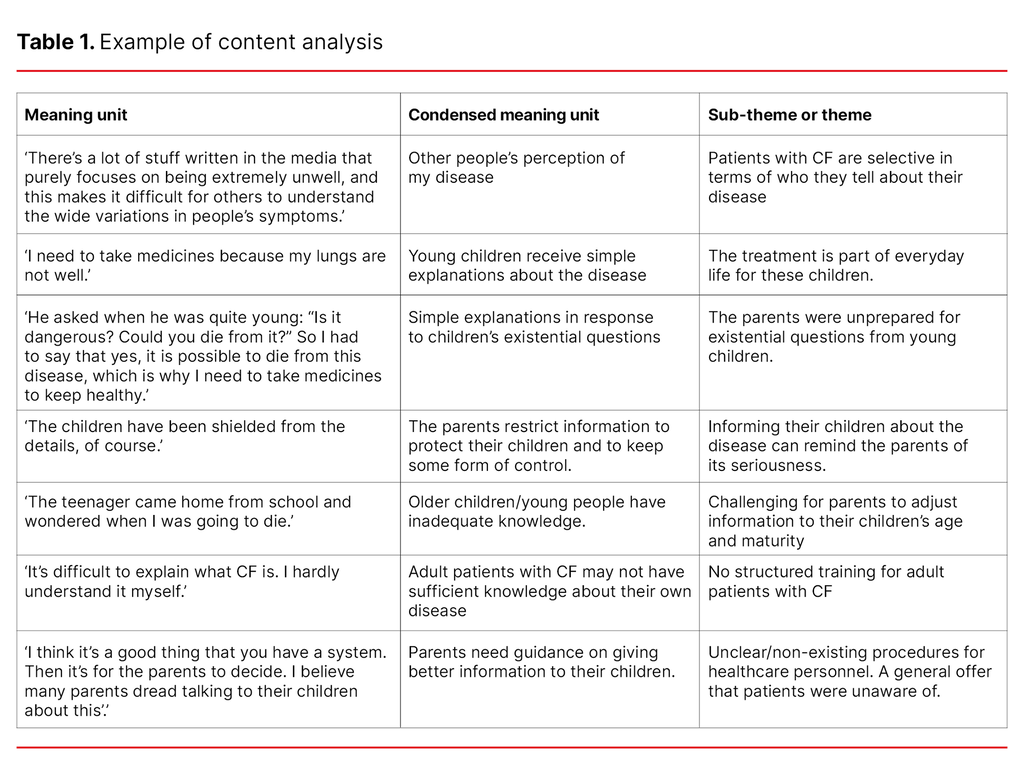
The units were then condensed and re-phrased, to allow the key content to emerge as condensed meaning units. We proceeded to group these units into categories, so that underlying meanings and core concepts formed sub-themes and themes, as demonstrated in Table 1. The first and last author both took part in the analytic process.
The first author conducted the interviews and transcribed the recordings. She has experience of the patient group after many years of working in a clinical setting. The last author has extensive research experience and provided supervision and quality assurance of the analysis.
Ethical considerations
The patients received oral and written information about the study. It has been approved by the data protection officer at Oslo University Hospital and meets the requirements of voluntary participation, informed consent, and confidentiality (20). The Regional Committee for Medical and Health Research Ethics (REC) considered the study to be a quality improvement project (REC South East Norway, reference no. 2014/896).
Results
The sample included twelve women and four men. Most of them had a job, while some were students or economically inactive for health reasons. We identified four main themes that align with the study’s objective. The first theme concerns the stigma associated with the disease and the informants’ reluctance to talk about their disorder.
The two subsequent themes concern information provided by parents to their children, while the last theme is associated with expectations of the healthcare professionals. Illustrative quotes from participants are put in quotation marks followed by the informant number. We have not specified the informant’s sex as there were few male participants and therefore a risk they could be identified.
The stigma associated with the disease
All informants were open about their CF disease with close adult relatives. Several informants reported that when they were teenagers, few people outside of the family knew about the disease, and as adults several of them provided limited information to friends and colleagues: ‘There’s a lot of stuff written in the media that purely focuses on being extremely unwell, and this makes it difficult for others to understand the wide variations in people’s symptoms’ (no. 2).
They had no wish to be compared to those who were very unwell, because their condition would be considered more severe than it was. They perceived this to be stigmatising. Some said they have a pulmonary disease, but few of them used the word ‘CF’ or ‘cystic fibrosis’. One of them said: ‘It’s been my strategy not to say that much, yes, that’s been my coping mechanism’ (no. 15).
Although they did not say so explicitly, there is reason to believe that this general reluctance to talk about the disease may have affected what they communicated to their own children. The informants were selective in terms of who they informed about the disease.
Simple but challenging information to children below school age
All the informants described their lives as normal, despite frequent hospital check-ups and regular use of intravenous antibiotics at home. Treatments such as inhalations, pulmonary physiotherapy, pancreatic enzymes and antibiotics were a natural part of their children’s everyday lives: ‘It’s not a condition that suddenly arrives, it’s been there all the time’ (no. 6).
The children were given simple explanations if they raised any questions: ‘I need to take medicines because my lungs are not well’ (no. 6).
Such explanations became part of everyday conversations between children and parents, mainly between the child and the parent with CF. In this study there was no difference between the nature of the information provided depending on whether it was the mother or father who had the disease. Some said they had explained the disease in a simple way so as not to frighten the children. But this could also be a way of taking control: ‘He talks a lot, and he doesn’t need all the information. So I want to have some control over what he gets to know’ (no. 1).
If the children talked about their parent’s disease with other people, it was considered less of a stigma to have a pulmonary disease than CF. When the children asked ‘Is it dangerous? Can you die from it?’ (no. 14), it was difficult to answer because the parents were ill prepared for questions of this nature. Some of them chose to be honest with the child: ‘It is possible to die from this disease, which is why I need to take medicines to keep healthy’ (no. 14).
Others reported that they had said: ‘It’s not that dangerous’ (no. 13). This would typically happen if the disease was in a stable phase. When they were older, some of these children had confronted their parents about having played down the disease. Other informants consciously limited the information about their disease in order to protect the child, often based on personal experiences: ‘The children have been shielded from the details, of course. That worked for me and my parents’ (no. 15). They had themselves been shielded from receiving information about their own disease when they were young, and they continued this tradition with their own children, with the best of intentions.
The exchange of information between parents and children below school age took the form of parents responding to their children’s questions as part of their everyday conversations. The informants were unprepared for existential questions from young children.
Inadequate information provided to young people
As the children grew older, their need for more extensive and detailed knowledge would also grow. The informants rarely engaged with teenagers and young adults about the disease. This could be due to insufficient knowledge about their own disease or that they felt it was difficult to convey this information. One of the informants said: ‘It’s difficult to explain it to the children, I hardly understand it myself’ (no. 11).
The informants had not been alert to their children’s need for more detailed information as they grew older. If the children did not raise any questions, the informants would forget or avoid providing further details as the children grew. Several believed that they had mentioned to the children that the name of their disorder was CF, but the disease was never referred to as CF in day-to-day life.
Genetics is part of the curriculum in lower secondary school, and CF is an example of an inherited disease. Some of the children had been taught about CF at school, and one informant reported that her teenager had said: ‘People with CF die before adulthood, and they can’t have children. The teenager came home from school and wondered when I was going to die’ (no. 5).
Most of the informants had been unaware that this age group are taught about genetics at school. It was difficult for the parents to adjust information to their children’s age and level of maturity.
Expectations of the health service
Among those in a stable condition and with a normalised daily life, most did not find it difficult to talk to their children. However, they felt it was more difficult to inform them about the seriousness of the disease and about the outlook for the future. All of them were confident that they would receive assistance if they asked for it. The parents were nevertheless unaware of the fact that healthcare personnel have a duty to ensure that children receive information about their parents’ disease. Explaining a deteriorating condition to the children was challenging. A couple of the informants who had found themselves in such situations had asked healthcare personnel for assistance in explaining the situation. One of them said: ‘I want him to know. But it’s difficult because I don’t want to frighten him’ (no. 7).
After giving it some thought, several said that guidance would be good: ‘It would be nice to be able to discuss things with a nurse or someone else knowledgeable who has the right experience ’ (no. 7). Nevertheless, everyone felt that they themselves were best suited for this task: ‘I think it’s a good thing that you have a system. Then it’s for the parents to decide. I believe many parents dread talking to their children about this’ (no. 1).
The informants did not expect healthcare personnel to give them support with providing simple information. They wanted to provide this type of information themselves.
Discussion
This study is among the first to investigate how parents with CF experience informing their children about the disease. The results demonstrate that the informants, all of them parents with CF, are selective in terms of who they tell about their disease. Young children received information when they asked questions in casual conversations with their parents.
This information was not adjusted as the children grew older. The parents were unprepared for existential questions from young children. They did not know that healthcare personnel have a duty to ensure that children receive information about the disease.
People with CF are selective in terms of who they tell about the disease
The parents reported that they felt ambivalent about informing other people about the disease, and that it was difficult to talk to others about its complexity. They described it as challenging for healthy people to understand that the morbidity varies from person to person. It was difficult to explain the nature of the disease and how hard people with CF are working to prevent the disease from progressing. To the outside world, it may seem as if people with CF live normal lives (21).
Earlier studies have also shown that people with CF are selective in terms of who they tell about their disease (21, 22). Situations that compel them to provide information about their disease can be tiered. The most demanding situations involve a fear of reactions and/or sanctions from the other person in response to the information they provide (22). This may potentially be the reason why some give their children incomplete information. Adults with CF may be lacking good knowledge about their own disease (23).
Communication as a concept involves some sort of communion, sharing something or having a connection with somebody else (24). The parents informed their children about CF in that the treatment was part and parcel of the daily routine. For the youngest children, this may well suffice. Young children need to know what is happening here and now. Children below school age have less of an ability to imagine what might happen in the distant future, for example that the disease may develop, or that the parents might die (11).
Good communication depends on intimacy, a good relationship and trust that the information brings something positive (24, 25). Our study describes the parents’ worry that the children may start to feel anxious if they are told about the parents’ disease. Older children and teenagers need to know about their parents’ outlook and the consequences of their disease. Inadequate knowledge about a parent’s disease may give rise to problems for older children and teenagers, who may come up with their own explanations (11), which are often worse than reality.
Better information from parents will prepare children and young people for any talk about the disease at school, or when they come across things on the internet. The study shows that the parents perceived older children to have insufficient knowledge about the disease. Earlier studies based on interviews with both parents and children (11) have shown that young people knew more about the parents’ disease than the parents were aware of, but this knowledge would often have shortcomings or involve misunderstandings.
Children raised existential questions for which the parents were unprepared
Existential questions concern suffering, death, meaning, freedom and loneliness (26). The study by Jessup et al. (27) showed that CF patients who wanted children considered it an ethical problem that their offspring might have CF. For some, the solution was not to have children of their own. Informing their children about the disease can be a reminder of its seriousness (25, 28).
Research in the field of cancer care shows that conversations about disease and death are difficult, both for patients and healthcare workers (11, 25, 28). When children choose not to ask about their parents’ disease, this can be seen as mutual protection. To protect the other party, parents withhold information while children withhold their worries (11, 29). This mutual protection can serve as a barrier to open dialogue within the family about emotional and existential themes.
Healthcare personnel were not expected to provide information to children about their parents’ illness
The informants were not aware that healthcare personnel have a duty to inform children about their parents’ illness. Parents who care for children must inform them of their own disease (8). The informants in this study felt that they were in the best position to inform their own children. Research also shows that parents are their children’s most important sources of information (11).
Our study shows how difficult it is for parents to inform their children about the disease in a way that is suited to the child’s age and level of maturity. Providing simple information to young children was not felt to be problematic. However, it appeared to be difficult for the parents to tell their children about the serious nature of the disease, and about the outlook for the future. The parents said they expected to receive assistance if they asked for it. Research on MS has shown that symptoms of anxiety and depression in parents have a direct impact on children’s mental behaviour, irrespective of the severity of the disease (13).
Other studies have shown that the children of chronically ill parents face a higher risk of behavioural problems (30). Good communication with the child and providing the child with information about the parent’s disease will probably reduce the child’s stress level (10). Hospital consultations constitute an arena where healthcare personnel can help parents to meet their children’s need for information. Information about the parents’ disease, and an open dialogue with the school, can prepare young people for school lessons in genetics (31). In our study, the parents with CF talked about older children who had lost their trust in their parents because they had been given inadequate information about the disease.
Strengths and weaknesses of the study
One of the study’s strengths was its qualitative design which allowed us to use the informants’ own experiences to shed light on the research questions. Information about sensitive and existential themes can be difficult to capture in a questionnaire. Whether the findings of this qualitative study are transferable to a wider population or to other chronic diseases is an important question. The generalisability is linked to the sample, but also to the question of relevance and how the findings can help shed light on a similar problem in a different context (21).
There is a considerable need to safeguard under-age relatives, including in the primary health service. There are currently no guidelines in place (32), but the findings of our study may help raise awareness of the problem. There are few similar studies, but research on cancer and MS patients may also be relevant to CF. While our study did not focus on the parents’ life-restricting disorder towards the end of their life, there are new recommendations in this field (33).
To bolster the validity of the study, we asked follow-up questions during the interviews in order to ensure that we had understood the informant correctly. The fact that the interviewer was a member of the therapeutic team may have posed a dilemma for the informants. However, earlier research has shown that familiarity with and trust in the interviewer can help with recruitment and lead to a more open dialogue (21). The fact that the children were not interviewed about their experiences was a weakness of this study.
Conclusion
Parents with CF need to know more about their own disease to be able to give their children better information. Measures should be put in place to ensure that children have a level of knowledge about their parents’ disorder which is appropriate for their age and maturity. Parents must be made aware of the duty that healthcare personnel have, and of their children’s rights in this respect.
The specialist health service must be more alert to their own responsibility to inform children about their parents’ disease and must seek to facilitate this in consultations with the parents. A safeguarding procedure should be drawn up for the children of chronically ill parents. Healthcare personnel need better competence in this field.
We are grateful to the patients who took part in the study, and to the National Centre for Cystic Fibrosis (NSCF) for giving us the opportunity to carry out the project.
The authors declare no conflicts of interest.
Open access CC BY 4.0.
The Study's Contribution of New Knowledge






Comments