Readmission of patients to the intensive care unit – a case-control study
Summary
Background: International studies show that readmission to the intensive care unit can result in higher mortality rates as well as reducing preparedness and increasing hospital costs. Readmission frequency is documented in Norwegian data registries, but little is known about what transfer characteristics typify readmitted patients.
Objective: The objective of the study was 1) to describe who is readmitted to a Norwegian intensive care unit, and 2) to compare transfer characteristics in relation to patients readmitted within 72 hours with patients who were not readmitted.
Method: A quantitative study with a case-control design. Data from the Norwegian Intensive Care Registry (NIR) identified all patients admitted to an intensive care unit at a university hospital in the period from 1 January 2014 to 31 December 2016. Forty-five patients were readmitted within 72 hours. Of these, forty-four patients were compared with a control patient who had been admitted to the same intensive care unit but had not been readmitted. The case control patients were matched according to age, reason for admission, disease severity score, nursing needs score, type of respiratory support and length of stay in the intensive care unit. Logistic regression analysis was used to calculate the odds ratio for readmission according to transfer characteristics.
Results: Of 1387 patients admitted during the study period, 105 (7.6%) were readmitted during the same hospital admission and 45 (32%) within 72 hours. Readmitted patients are older, but their mortality rate is almost equal to that of non-readmitted patients. The patients readmitted within 72 hours have a significantly higher likelihood of having an incomplete written transfer report (odds ratio [OR] 5.12, p < 0.001).
Conclusion: Incomplete written transfer reports result in a significantly higher likelihood of readmission. Studies should be conducted with a larger sample in order to shed more light on the findings of the study.
Cite the article
Naustdal K, Drageset J. Readmission of patients to the intensive care unit – a case-control study. Sykepleien Forskning. 2020;15(80647):e-80647. DOI: 10.4220/Sykepleienf.2020.80647en
The intensive care unit (ICU) treats the most severely ill patients in the hospital – patients with single or multiple organ failure (1). Since the treatment requires advanced equipment and drugs as well as continuous monitoring, ICU beds represent an expensive and limited resource (2).
A limited capacity may result in some patients being transferred to a ward prematurely. The assessment is based not only on the patient’s medical condition but also on other patients’ need for an ICU bed.
Differences in readmissions internationally and in Norway
Various checklists are used internationally to evaluate admission and discharge from the ICU, but we do not know whether they reduce readmissions (3). Moreover, even though a checklist is available, it has been demonstrated that this is seldom used (4).
As far as we are aware, checklists are not used on discharge from Norwegian ICUs. Consequently, ICU nurses and doctors perform a professional but subjective assessment in each individual case.
A number of the patients who are transferred are sent back to the ICU. International studies show that between 5.3 and 7.4 per cent of the patients who are discharged from the ICU are readmitted during the same hospital admission (5, 6), and between 3 and 3.8 per cent of the patients are readmitted within 72 hours of transfer to a ward (7, 8).
What does readmission entail?
Readmission to an ICU presents a complex challenge on several levels. For the patient it leads to a longer period of illness and increased mortality (5, 6, 9). In addition, preparedness may be reduced in the ICU, which entails increased costs for society (10).
The patients who are readmitted most often suffer from respiratory failure, circulatory failure or sepsis (5, 9). They are often older and are more likely to have single or multiple medical diagnoses; they have had emergency surgery as opposed to elective surgery, a higher disease severity score, increased comorbidity and a longer first stay in the ICU (5).
There can be many reasons for readmission. Ventilator treatment for 24 hours or more, a short time from extubation (the tracheal tube is removed from the patient’s airways) to the time of transfer, or a considerable need for oxygen at the time of transfer, may be associated with increased risk of readmission (11).
According to Elliott et al., an association has been found between transfer ‘out of hours’ and the risk of readmission (5).
The patient may experience transfer to a ward as one of the more stressful aspects of the ICU stay (12, 13). Although there are a number of contributory factors, patients, their families and ICU nurses identify communication between the ICU and the ward as a weak point (9).
The lack of communication or misunderstandings can lead to adverse events for the patient (14). On this basis, the World Health Organization (WHO) has recommended using structured reporting (15).
A number of studies focus on the effect of introducing various interventions such as a transfer form or a liaison nurse (16). The results are not conclusive.
Objective of the study
Even though there have been many international studies on readmission to the ICU, and the Norwegian Intensive Care Registry reveals a high incidence of readmissions to Norwegian ICUs, we have little knowledge of whom this applies to or what causal relationships exist in a Norwegian context.
The objective of this study was therefore to describe the patients who are readmitted to a Norwegian ICU and to investigate whether the transfer characteristics related to patients who are readmitted within 72 hours differ from those of patients who are not readmitted.
Method
Study setting
The study was conducted at a university hospital that treats approximately 800 000 patients annually. The ICU in question is one of six ICUs at the hospital and can treat eleven patients of all ages with various surgical and medical diagnoses.
In line with the European standard, the unit is classified as a Level 3 unit, i.e. it has the highest level of expertise and treatment options (1).
The unit is organised as a closed ICU where specialist ICU doctors are in charge of the treatment. The patients receive 24-hour one-to-one nursing care, and the coverage rate of intensive care nurses is over 98 per cent.
Data collection
When an intensive care patient is hospitalised in the ICU, data and values that describe the treatment and care are collected and registered in an electronic patient chart and the patient record. Some of the data are also registered in NIR (17) via the Norwegian Health Net and the medical registration platform (18).
Sample
All the patients admitted to the ICU in question in the period from 1 January 2014 until 31 December 2016 were identified via NIR. According to NIR, 141 patients were readmitted during the study period. However, some of these patients proved not to have been readmitted in reality.
These cases related to errors in NIR’s data plotting (24 patients), one planned readmission and eleven patients who were transferred to another ICU because of capacity problems. These 36 patients were excluded from the study.
The remaining 105 patients were included in the first part of the study. Forty-five of these were readmitted within 72 hours of the transfer to a ward. One patient had no matching control subject and was excluded.
Patients with treatment restrictions or who died within 72 hours of the transfer were excluded from the control group.
Consequently, we included 44 patients in both the case group and the control group in the second part of the study.
With 44 cases and 44 controls and a prevalence of exposure varying from 10 to 50 per cent in the control group, there is an 80 per cent statistical power to detect an odds ratio of 3.6–4.6 as statistically significant if the significance level is set at 5 per cent.
Variables
From NIR (19), we obtained mortality rates and demographic variables such as age and gender for all patients included in the study. Information about admission and discharge times, and the reason for admission and readmission, was obtained from the electronic patient charts and patient journals.
Values describing the degree of severity of the illness and care needs in the form of SAPS II (Simplified Acute Physiology Score II), SOFA (Sequential Organ Failure Assessment score) and NEMS (Nine Equivalents of Nursing Manpower Use Score) were obtained from NIR and checked against the electronic patient charts.
For patients who were readmitted within 72 hours, we also obtained information from the electronic patient charts about respiratory support and the interval between the last treatment (invasive care or non-invasive care) and transfer.
The content of the written transfer report was obtained from the patient record. In this study, we defined a complete written transfer report as a written report from both the ICU nurse and doctor that included guidelines or recommendations for further treatment in accordance with the unit’s procedures and the recommendations of the guidelines for intensive care in Norway (1).
Study design and procedure
The second part of the study was carried out retrospectively with a case control design. The 44 patients were matched one on one with a case control patient who had been admitted to the same ICU but who had not been readmitted.
The case group and control group were matched in terms of age, SAPS II and NEMS because these factors are significantly associated with greater risk of readmission and increased mortality (5). Moreover, we matched the patients in terms of reason for admission, respiratory support and length of stay. All the information was obtained from the first ICU stay.
For each case, the relevant control patients were manually sorted into a prioritised order according to the following criteria: age ranges (±10 years), reason for admission, closest possible SAPS II (±21) (20), closest possible NEMS (±12) (20) and respiratory support in the form of invasive or non-invasive ventilation.
Furthermore, the patient with the closest possible length of stay (±9.4 days) was chosen as a match.
The SAPS II scores of four of the patients included showed variation greater than 9. Nevertheless, they were included since their SOFA scores were approximately the same on transfer to the ward (±2) (21). For three of the patients, there was no match with respiratory support.
We decided therefore to match these patients with a control patient who had received ventilator treatment for a short period (±4.8 hours).
The main purpose of the study was to examine whether various transfer characteristics that could be linked to the first ICU stay affected the likelihood of readmission. Hence we wanted the groups to be as similar as possible in terms of patient-specific factors that could influence the risk of readmission.
Ethics
The study has been assessed by the Regional Committees for Medical and Health Research Ethics (REC) and defined as a quality assurance project (reference number 2017/1313) (22). The study is approved by departmental management and the hospital trust’s data protection officer has agreed to the data collection (reference number 2017/12493).
The study was also approved by NIR, which is exempt from the informed consent requirement of the Norwegian Centre for Data Research (reference number 2009/7537). All patients or their families received written information stating that data from the ICU stay were collected and stored anonymously in a database, and the data could be utilised later for research purposes.
Information was also given about disclosure and the right not to participate. This study will have no impact on the patients included, since we studied secondary data.
Analysis
The Stata 15 statistical software package was used to analyse the data. Continuous variables (age, length of stay) are described using mean and standard deviation. Categorical variables (gender, mortality, reasons for admission) are described in numbers (n) and percentages (%).
Significance was tested using a two-sample t-test (age) and chi-square test for categorical variables (gender and mortality). The significance level was set at 5 per cent, corresponding to p-value <0.05 (Table 1).
We used unadjusted (Model 1), partly adjusted (Model 2) and fully adjusted (Model 3) logistic regression analysis (odds ratio [OR]) to calculate the likelihood of readmission in relation to the transfer characteristics.
Model 2 uses conditional logistic regression analysis with an adjustment for the variables used in the match (age, gender, SAPS II, NEMS, length of stay) (23) in order to assess whether the matching with the case control group was satisfactory and to examine whether gender was of significance for the likelihood of readmission.
Model 3 is adjusted for the transfer characteristics that we studied. Model 3 is only presented in Table 2, since these findings will be identical in all analyses. The dependent variable is readmission within 72 hours.
The variables were dichotomised for the adjusted analyses as follows: case control: non-readmitted patient = 0, readmitted patient = 1. Gender: female = 1, male = 2. Respiratory support: more than 24 hours between the last treatment and the transfer = 0, less than 24 hours between the last treatment and transfer = 1.
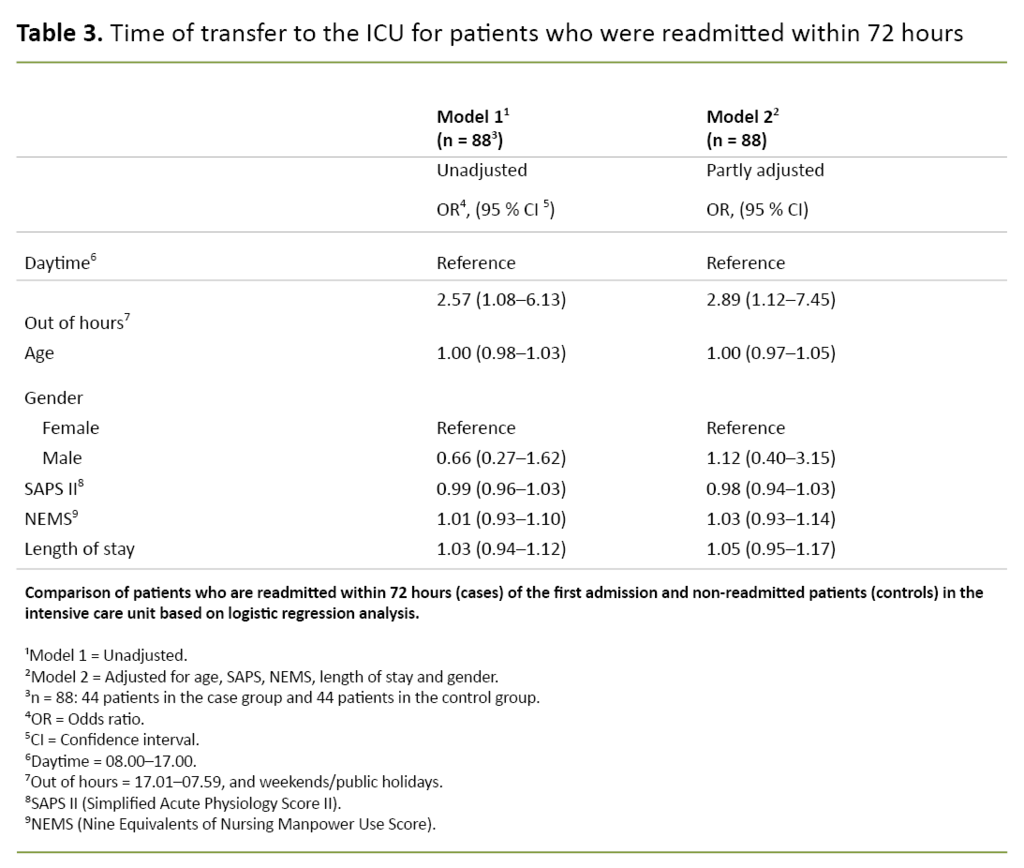
Time of transfer: daytime (08.00–17.00) = 0, ‘out of hours’ (17.01–07.59) and weekends/public holidays = 1. Transfer report: complete transfer report (written transfer report from both the ICU nurse and the ICU doctor including guidelines and recommendations on further treatment) = 0, incomplete transfer report (one or more instances of missing data in the complete transfer report) = 1 (Tables 2, 3 and 4).
Missing data
Four patients had no SAPS II values. They were matched according to NEMS. One of the reasons for the absence of SAPS II is that this is not calculated for children under the age of 16 (17).
Results
During the study period, 1387 patients were admitted to the ICU in question. Of these, 105 patients (7.6%) were readmitted during the hospital stay, and 45 patients (3.2%) were readmitted within 72 hours of transfer from the ICU.
Over 60 per cent of those who were readmitted were men.
The patients who were readmitted were aged between 0 and 83 years and the mean age was 57.7 years. Patients who were readmitted within 72 hours were older, but the difference was not statistically significant (59.6 years, p = 0.054). Over 60 per cent of those who were readmitted were men (Table 1).
Reasons for admission and readmission
Patients who were readmitted (n = 105) had the following organ failure on readmission: respiratory failure (63%), neurological failure (11%) and circulatory failure (10%), followed by organ injury or trauma, sepsis and gastrointestinal failure (data not shown in the tables).
Patients who were readmitted within 72 hours had been first admitted with the following: respiratory failure (41%), neurological failure (30%), circulatory failure (16%), organ injury or trauma (9%), sepsis (2%) and gastrointestinal failure (2%).
The main reasons for readmission were as follows: respiratory failure (60%), neurological failure (13%), circulatory failure (13%) and gastrointestinal failure (7%). Other reasons included sepsis, haematologic failure and following different kinds of surgery (data not shown in the tables).
Length of stay in the ICU and hospital
The patients (n = 105) who were readmitted had a somewhat longer, though not significantly longer, length of stay in the ICU during their first ICU admission.
The mean length of stay for readmitted patients (n = 105) was 5.3 days (standard deviation [SD]: 5.6, p = 0.738) and 5.5 days (SD: 5.2, p = 0.697) for patients readmitted within 72 hours (n = 45) (data not shown in the tables).
Patients readmitted within 72 hours had a mean average ventilator time of 3.2 days (SD: 4.1) during their first stay, and a mean SAPS II score of 42.6 (SD: 12.7) (data not shown in the tables).
Mortality
Patients readmitted within 72 hours had a lower 90-day mortality rate (15.5%) than patients who were not readmitted (26%), but the difference is not significant (Table 1).
Transfer characteristics
Patients who received respiratory support in the 24 hours prior to transfer were twice as likely to be readmitted (OR 1.09) (Table 2). In unadjusted analysis (Table 3), the likelihood of being transferred ‘out of hours’ was more than two and a half times higher when compared with non-readmitted patients (OR 2.57).
Patients with incomplete written transfer reports were five times as likely to be readmitted.
Patients with incomplete written transfer reports were five times as likely to be readmitted (OR 5.12).
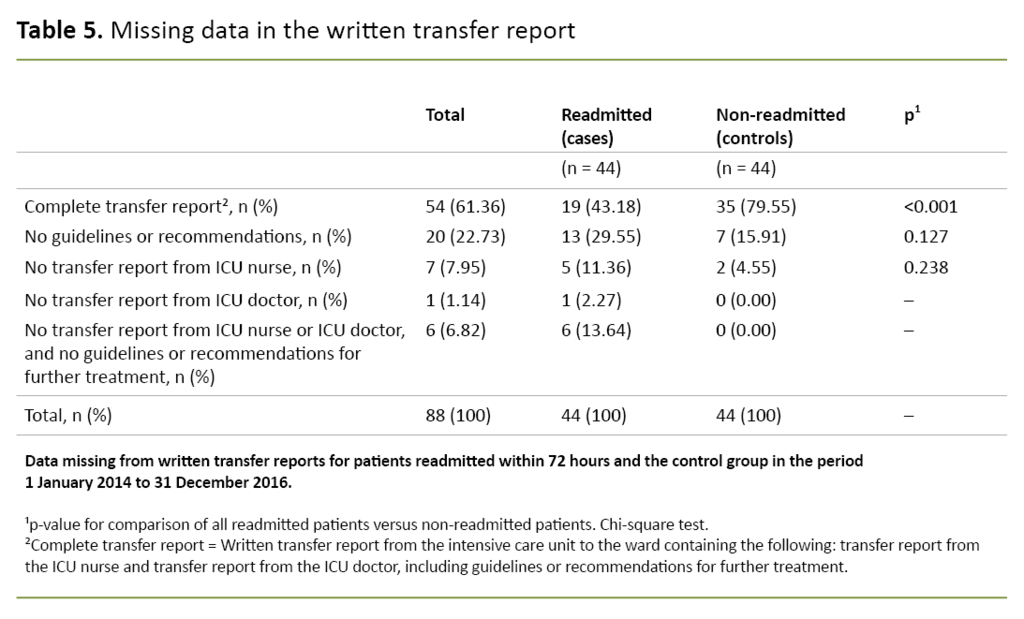
The correlation between an incomplete written transfer report and readmission remains significant after adjustment for age, gender, SAPS II and NEMS (p < 0.001) (Table 4). The missing data in the transfer report are presented in a separate table (Table 5).
Discussion
In this study, we found that intensive care patients who were readmitted were somewhat older than non-readmitted patients but that mortality rates were very similar. Intensive care patients who were readmitted within 72 hours were over 2.5 times more likely to have been transferred ‘out of hours’.
The patients were also over five times more likely to have an incomplete transfer report compared with equally ill patients who were not readmitted.
Percentage of readmitted patients
The mapping of readmitted patients shows a readmission rate of 7.6 per cent during the hospital stay and 3.2 per cent during the first 72 hours after discharge. This result corresponds with earlier findings (5–8).
Earlier studies show that the patients who are readmitted are older than those who are not readmitted, that there is a preponderance of men and that most are readmitted with respiratory failure (5, 7, 9, 24).
Mortality among readmitted patients
In contrast to other studies (5. 6), our findings show that readmission is not significantly associated with mortality. The patients who were readmitted within 72 hours had a lower 90-day mortality rate (15.5 per cent) than those who were not readmitted (26 per cent), but the difference was not significant.
In contrast to other studies, our findings show that readmission is not significantly associated with mortality.
One possible explanation of this finding is the small sample in the study. Other possible explanations may be that there was a lower threshold for readmitting children, and the inclusion of children in the study resulted in a reduction in mortality. The older the patient, the greater the likelihood of a shorter survival period.
Earlier studies show that older patients have a shorter length of stay in the ICU, higher mortality and a higher incidence of death in the ward than in the ICU (25). The university hospital in question has several intermediate care units, and in some cases the patients were placed in such units instead of being readmitted to the ICU.
The limited intensive care capacity of the university hospital may entail frequent, systematic assessment of the treatment level they can offer patients, with discussion of limitation of intensive care as part of the future care plan. Terminally-ill patients may therefore not be offered another stay in the ICU.
In our study, we found that patients had a significantly higher likelihood of readmission if they were transferred ‘out of hours’, a finding which corresponds with earlier studies (5).
Transfer report
This study shows that patients who were readmitted within 72 hours were five times more likely (OR = 5.1, p < 0.001) to have an incomplete transfer report compared with patients who were not readmitted (Table 3).
During a hospital stay, patients can experience being moved between various units several times. All transfers pose a risk to the patient in that poor communication or misunderstandings may lead to adverse events (14, 16, 26).
Since inadequate communication can lead to a lack of continuity in care, wrong treatment and potential injury to the patient, the WHO has recommended the use of structured reporting (15). No such instrument has been implemented at the ICU in question.
Earlier studies did not find an association between different transfer practices, including written communication and readmission or mortality, but indicate that local conditions can provide insights that may improve transfer practices (27).
Several patients with incomplete transfer reports lacked a written transfer report from the ICU nurse (Table 5). Even though transfer between the ICU and the ward is almost a daily procedure, no transfer situations are identical.
Findings in the study may indicate that the guidelines were not always complied with in connection with the transfer.
The ICU in question had its own procedure for transferring patients to a ward, but findings in the study may indicate that the guidelines were not always complied with in connection with the transfer.
One possible explanation may be that the ICU nurse must quickly make preparations for a new patient, and consequently, the written transfer report may be cursory or forgotten because of a high workload.
Lack of guidelines and recommendations for further treatment
The most common limitations of the transfer report identified in our study related to a lack of guidelines or recommendations for further care and treatment (Table 5). Earlier studies indicate that patients do not always receive the necessary follow-up in the ward (11).
An incomplete written transfer report in which guidelines and recommendations are not given can make it challenging for registered nurses (RNs) in the ward to assess what monitoring and treatment should be prioritised.
Earlier research shows that a written summary of the patient care pathway can be an important communication tool that presents and prioritises information systematically and thus highlights the challenges faced by the patient (28). Patients who are transferred from an ICU to a ward have serious and often complex illnesses that demand a high level of competence from the RNs in the ward.
Earlier studies have shown an inadequate level of knowledge among RNs in the ward (9), which may pose a barrier to acquiring a complete overview of these patients’ situation. Consequently, the lack of guidelines and recommendations for further treatment can make the RNs less able to give the patient the necessary follow-up, which may lead to a greater number of readmissions.
Other circumstances related to the transfer may also affect readmission. Van Sluisveld et al.’s literature review (16) emphasises that nursing culture, teamwork and oral reporting are important factors that prevent correct patient transfer.
It was not possible to examine these factors in our study since it had a retrospective design. Nor was the objective of the study to assess all aspects of the communication but to describe their association with readmission.
Strengths and weaknesses of the methodology
A strength of the study is that the patients are matched and are as similar as possible in terms of patient specific factors. Consequently, it is not the severity of the illness that leads to differences in respect of the case control group.
Since this is a small study, it is possible that weaker associations may wrongly appear as non-significant due to a lack of statistical power.
The study has several weaknesses. A retrospective design means that it is not possible to investigate why patients are transferred, what the reasons are for incomplete written transfer reports or what other factors play a role, such as oral transfer reporting.
We had a small sample from one single unit at one hospital. The findings are therefore not necessarily representative of other units and in other settings.
Conclusion
The study showed that patients who were readmitted had a significantly higher (p < 0.001) likelihood of having incomplete written transfer reports compared with patients who were equally ill but who were not readmitted.
The study also showed that there should be greater focus on ensuring good transfer documentation, particularly the dissemination of further follow-up measures.
Studies should be conducted with a larger sample in order to shed more light on the findings of our study and to explore measures that could reduce the number of readmissions.
We wish to express our gratitude to the ICU in the study. Thanks to Dr.med Reidar Kvåle and ICU nurse Britt Sjøbø for assistance in designing and carrying out the study. Thanks also to Senior Engineer Jannicke Igland at the Department for Global Public Health and Primary Care at the University of Bergen for her advice and help in connection with statistical analyses.
References
1. Norsk Anestesiologisk Forening, Norsk sykepleierforbunds landsgruppe av intensivsykepleiere. Retningslinjer for intensivvirksomhet i Norge. Oslo; 2014. Available at: https://www.nsf.no/Content/2265711/Retningslinjer_for_IntensivvirksomhetNORGE_23.10.2014.pdf (downloaded 17.10.2017).
2. Stubberud DG. Utskriving fra intensivavdeling. In: Gulbrandsen T, Stubberud DG, eds. Intensivsykepleie. 3rd ed. Oslo: Cappelen Damm Akademisk; 2015. p. 296–310.
3. Gajic O, Malinchoc M, Comfere TB, Harris MR, Achouiti A, Yilmaz M. The Stability and Workload Index for Transfer score predicts unplanned intensive care unit patient readmission: initial development and validation. Crit Care Med. 2008 mars;36(3):676–82.
4. Smischney NJ, Cawcutt KA, O’Horo JC, Sevilla Berrios RA, Whalen FX. Intensive care unit readmission prevention checklist: is it worth the effort? Journal of Evaluation in Clinical Practice. 2014 april;20(4):348–51.
5. Elliott M, Worrall-Carter L, Page K. Intensive care readmission: a contemporary review of the literature. Intensive Crit Care Nurs. 2014 Jun.;30(3):121–37.
6. Wong EG, Parker AM, Leung DG, Brigham EP, Arbaje AI. Association of severity of illness and intensive care unit readmission: a systematic review. Heart & Lung – The Journal of Acute and Critical Care. 2016 Jan.–Feb.;45(1):3–9.e2.
7. Makris N, Dulhunty J, Paratz J, Bandeshe H, Gowardman J. Unplanned early readmission to the intensive care unit: a case-control study of patient, intensive care and ward-related factors. Anaesthesia and Intensive Care. 2010 Jul.;38(4):609–794.
8. Wagner J, Gabler NB, Ratcliffe SJ, Brown SE, Strom BL, Halpern SD. Outcomes among patients discharged from busy intensive care units. Ann Intern Med. 2013 Oct.; 159(7):447–55.
9. Russell S. Reducing readmissions to the intensive care unit. Heart & Lung – The Journal of Acute and Critical Care. 1999 Sep.–Oct.;28(5):365–72.
10. Kramer AA, Higgins TL, Zimmerman JE. The association between ICU readmission rate and patient outcomes. Crit Care Med. 2013 Jan.;41(1):24–33.
11. Elliott M. Readmission to intensive care: a review of the literature. Austr Crit Care. 2006 august;19(3):96–104.
12. Cypress BS. Transfer out of intensive care: an evidence-based literature review. Dimensions of Critical Care Nursing. 2013 Sep.–Oct.;32(5):244–61.
13. Chaboyer W, Kendall E, Kendall M, Foster M. Transfer out of intensive care: a qualitative exploration of patient and family perceptions. Austr Crit Care. 2005 Nov.;18(4):138–145.
14. Wong MC, Yee KC, Turner P. Clinical handover literature review. University of Tasmania, Australia: Australian Commission on Safety and Quality in Healthcare; 2008. Available at: https://www.safetyandquality.gov.au/wp-content/uploads/2008/01/Clinical-Handover-Literature-Review-for-release.pdf (downloaded 12.01.2018).
15. Verdens helseorganisasjon (WHO). Patient safety solutions: communication during patient handovers. Genève: The Joint Commission International; 2007. Available at: http://www.who.int/patientsafety/solutions/patientsafety/PS-Solution3.pdf (downloaded 14.01.2018).
16. van Sluisveld N, Hesselink G, Hoeven J, Westert G, Wollersheim H, Zegers M. Improving clinical handover between intensive care unit and general ward professionals at intensive care unit discharge. Intensive Care Medicine. 2015 Feb.;41(4):589–604.
17. Helse Bergen. Data i Norsk intensivregister [Internet]. Bergen; 2017 [published 19.05.2017; updated 19.05.2017; cited 10.05.2018]. Available at: https://helse-bergen.no/norsk-intensivregister-nir/data-i-norsk-intensivregister
18. Helse Bergen. Historikk [Internet]. Bergen; 2017 [published 19.05.2017; updated 19.05.2017; cited 10.05.2018]. Available at: https://helse-bergen.no/norsk-intensivregister-nir/historikk
19. Helse Bergen. Norsk intensivregister [Internet]. Bergen; s.a. [updated 18.02.2018; cited 10.05.2018]. Available at: http://www.intensivregister.no
20. Haagensen R, Jamtli B, Moen A, Stokland O. Virksomhetsregistrering ved intensivavdelinger. Tidsskrift for Den norske legeforening. 2001 Feb.;121(6):687–90.
21. Vincent JL, Moreno R, Takala J, Willatts S, De Mendonça A, Bruining H, et al. The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. Intensive Care Medicine. 1996 juli;22(7):707–10.
22. Regionale komiteer for medisinsk og helsefaglig forskningsetikk. Available at: https://helseforskning.etikkom.no/ikbViewer/page/forside?_ikbLanguageCode=n (downloaded 12.05.2018).
23. Pearce N. Analysis of matched case-control studies. The BMJ. 2016;352:i969. DOI: 10.1136/bmj.i969
24. Ho KM, Dobb GJ, Lee KY, Finn J, Knuiman M, Webb SA. The effect of comorbidities on risk of intensive care readmission during the same hospitalization: a linked data cohort study. J Crit Care. 2009 mars;24(1):101–7.
25. Andersen FH, Kvale R. Do elderly intensive care unit patients receive less intensive care treatment and have higher mortality? Acta Anaesthesiologica Scandinavica. 2012 Nov.;56(10):1298–305.
26. Niven DJ, Bastos JF, Stelfox HT. Critical care transition programs and the risk of readmission or death after discharge from an ICU: a systematic review and meta-analysis. Crit Care Med. 2014 Jan.;42(1):179–87.
27. van Sluisveld N, Bakhshi-Raiez F, de Keizer N, Holman R, Wester G, Wollersheim H, et al. Variation in rates of ICU readmissions and post-ICU in-hospital mortality and their association with ICU discharge practices. BMC Health Services Research. 2017 Apr.;17(1):281–93.
28. Stelfox HT, Lane D, Boyd JM, Taylor S, Perrier L, Straus S, et al. A scoping review of patient discharge from intensive care: opportunities and tools to improve care. Chest. 2015 Feb.;147(2):317–27.
The following sentence has been corrected 8. December 2022:
Van Sluisveld et al.’s literature review (16) emphasises that nursing culture, teamwork and oral reporting are important factors in ensuring correct patient transfer.
It has been corrected into this:
Other circumstances related to the transfer may also affect readmission. Van Sluisveld et al.’s literature review (16) emphasises that nursing culture, teamwork and oral reporting are important factors that prevent correct patient transfer.



Comments