First-time mothers’ knowledge of pelvic floor muscle training and postnatal follow-up of pelvic floor function
Summary
Background: The strain placed on the pelvic floor during pregnancy and childbirth can impair its supportive function. Injuries to the pelvic floor muscles can be prevented or treated to some extent through pelvic floor muscle training (PFMT). Various studies show that individualised postnatal follow-up of pelvic floor function yields better outcomes than unsupervised training. Guided PFMT often improves technique, and thereby effectiveness. Adequate knowledge and guidance are essential to ensure correct performance of the exercises.
Objective: To examine the association between receiving information and follow-up during antenatal and postnatal care and first-time mothers’ knowledge of PFMT. We also aimed to assess whether healthcare personnel monitor pelvic floor function after childbirth.
Method: A cross-sectional study with data collected anonymously via an online questionnaire. First-time mothers aged >18 years who gave birth in Norway between 1 January 2022 and 1 July 2023 were included (n = 1093). Data were analysed using descriptive statistics and Pearson’s chi-square test.
Results: Only 40% of respondents reported receiving information on PFMT during pregnancy or the postnatal hospital stay, and only 30% discussed PFMT at the postnatal check-up. Women received inconsistent information on PFMT and follow-up regarding pelvic floor function during pregnancy, the postnatal hospital stay and at the postnatal check-up. Participants indicated that the postnatal check-up focused mainly on sexual health and contraception, with few receiving information on pelvic floor–related issues. A substantial proportion of women felt that the information provided as part of their antenatal and postnatal care was inadequate to perform PFMT unsupervised.
Conclusion: Few women reported receiving information on PFMT during pregnancy or the postnatal hospital stay or at the postnatal check-up. Although many acquired knowledge independently and attended postnatal consultations, few sought further follow-up from healthcare personnel. These findings highlight the need for better postnatal follow-up of pelvic floor function.
Cite the article
Bartok N, Eidesmo J, Nedberg I. First-time mothers’ knowledge of pelvic floor muscle training and postnatal follow-up of pelvic floor function. Sykepleien Forskning. 2025;20(102442):e-102442. DOI: 10.4220/Sykepleienf.2025.102442en
Introduction
The Norwegian Directorate of Health recommends that women be provided with information on pelvic floor muscle training (PFMT) as part of their antenatal care (1). National clinical guidelines for postnatal care strongly advise one to two structured, individualised consultations during their postnatal hospital stay, including information and guidance on pelvic floor muscles and the offer of tailored exercise programmes (2).
In these guidelines (2), less emphasis is placed on the recommendation for women to undergo a postnatal check-up with a doctor or midwife 4–6 weeks after childbirth. The purpose of the check-up is to identify any need for further follow-up, and it should address issues such as pelvic pain, incontinence, assessment of perineal lacerations and sexual health (2).
Understanding the importance of providing information and guidance on pelvic floor muscles before and after childbirth requires knowledge of their anatomy and function. The pelvis is closed inferiorly by muscles that form the pelvic floor. The deep muscles of the pelvic floor are essential for supporting the vagina, uterus, ovaries, bladder and rectum, ensuring optimal organ function. The pelvic floor also contributes to the regulation of intra-abdominal pressure during actions such as jumping, sneezing or laughing (3).
During pregnancy, the uterus increases in size, placing greater pressure on the pelvic floor (4). During vaginal delivery, the pelvic floor muscles are stretched to more than three times their resting length (5). The strain during pregnancy and childbirth can cause overstretching and tearing of muscle fibres and nerves, which can compromise the supportive function of the pelvic floor (6).
When the pelvic floor muscles are weakened or injured, the physical consequences include urinary incontinence, anal incontinence and pelvic organ prolapse, with the former being the most common. Several studies report that approximately 30% of women experience urinary incontinence for up to four years after childbirth (7–9).
As with other skeletal muscles, the pelvic floor requires training to maintain or increase its strength and supportive function. The recommendation for strengthening the pelvic floor after childbirth is pelvic floor contractions for six to eight seconds, eight to twelve times per session, three times daily (3).
Women are advised to perform PFMT for three to six months postpartum and to continue the exercises a few times each week for the rest of their life (6).
Evidence regarding PFMT as a preventive or therapeutic intervention for pelvic floor–related disorders associated with pregnancy and childbirth is mixed. However, there is consensus that PFMT is effective in both preventing and treating urinary incontinence (10, 11).
The effect of PFMT on faecal incontinence remains uncertain (7). PFMT can also be recommended as a conservative strategy to reduce symptoms of pelvic organ prolapse (12). Effective training requires women to learn how to correctly identify and activate the pelvic floor muscles, which can be challenging without individualised guidance (11, 13–15).
Several high-income countries have studied women’s experiences of receiving information and follow-up regarding PFMT, but we have not found any studies with a focus on the Norwegian context.
New national guidelines for maternity care in Norway were published after this study was completed, but they do not address PFMT. Consequently, recommendations on PFMT continue to be based on the current national guidelines for antenatal (1) and postnatal care (2).
Objective of the study
The aim of this study was to investigate the following research question:
What is the association between receiving information and follow-up during antenatal and postnatal care and first-time mothers’ knowledge of PFMT and postnatal follow-up of pelvic floor function by healthcare personnel?
The specific research questions were as follows:
- What proportion of women receive information on PFMT during pregnancy, the postnatal hospital stay and at the postnatal check-up?
- What information do women receive regarding PFMT and the follow-up of pelvic floor function during pregnancy, the postnatal hospital stay and at the postnatal check-up?
- To what extent do women feel they have sufficient knowledge to maintain pelvic floor function based on the information and follow-up they have received?
Method
The data in this cross-sectional study were collected anonymously via questionnaire. The study population comprised first-time mothers who gave birth between 1 January 2022 and 1 July 2023, at ≥ 37 weeks of gestation.
First-time mothers were selected to ensure a comparable baseline regarding the information received on PFMT. The study period was chosen to minimise the risk of recall bias. All modes of delivery were included to enable comparison of the information provided to different groups.
A self-selected, non-probability sampling method was used. Given our limited resources, this method was considered easier, quicker and more cost-effective for recruiting participants. Recruitment was via the social media platforms Facebook and Instagram.
A post that could be shared publicly was created and published in national and local Facebook groups, including due-date and postnatal groups, and through Instagram profiles that could reach the target population. The post included a link to the study website. Information about the study was shared multiple times during the recruitment period to increase participation. A total of 1093 participants were included in the study.
Questionnaire and variables
The digital questionnaire consisted of 26 questions covering sociodemographic characteristics, childbirth and information on PFMT during antenatal and postnatal care. No validated questionnaires directly addressing the research question were identified; therefore, the questions were partly self-developed and partly adapted from validated questionnaires in the Norwegian Institute of Public Health’s questionnaire bank (16).
This approach can potentially introduce information bias. To address potential issues with the self-developed questionnaire, a pilot study was conducted with 20 respondents. Their feedback led to us adding a ‘Don’t remember’ response option for several questions and the use of illustrations to describe perineal lacerations.
Analysis
Following data collection in the online survey tool Nettskjema, the dataset was exported to IBM SPSS Statistics version 29 and then screened for extreme values and obvious errors. Results for the first and second research questions were summarised as frequencies and percentages.
For the third research question, Pearson’s chi-square test was used to examine whether there was a statistically significant association between information on PFMT provided during the postnatal hospital stay and women’s evaluation of the adequacy of the overall information and follow-up of pelvic floor function.
The chi-square test yields a p-value, indicating the likelihood that an observed difference is due to chance. If the p-value is < 0.05, the null hypothesis is rejected. However, p-values alone do not fully reflect the scientific relevance of the findings.
Ethical considerations
The data collected did not include personally identifiable information, and background characteristics were reported in categories. Consequently, no assessment was required by Sikt – the Norwegian Agency for Shared Services in Education and Research (18). As the study was not intended to generate new knowledge on health or morbidity, approval by the Regional Committees for Medical and Health Research Ethics (REK) was deemed unnecessary (19).
The study was conducted in accordance with professional ethical guidelines for midwives, which outline the need for them to share evidence-based information and protect women’s privacy (20). The study also adhered to the Declaration of Helsinki, which underscores the importance of informed consent and places ethical responsibility on the researcher (21), in line with the Norwegian Research Ethics Act (22).
Results
A total of 1213 questionnaire responses were received, of which 1212 women had given birth in Norway within the specified study period. Thirty-eight respondents reported preterm delivery, and 81 were multiparous. These women did not meet the study’s inclusion criteria and were therefore excluded and not sent the remaining questions.
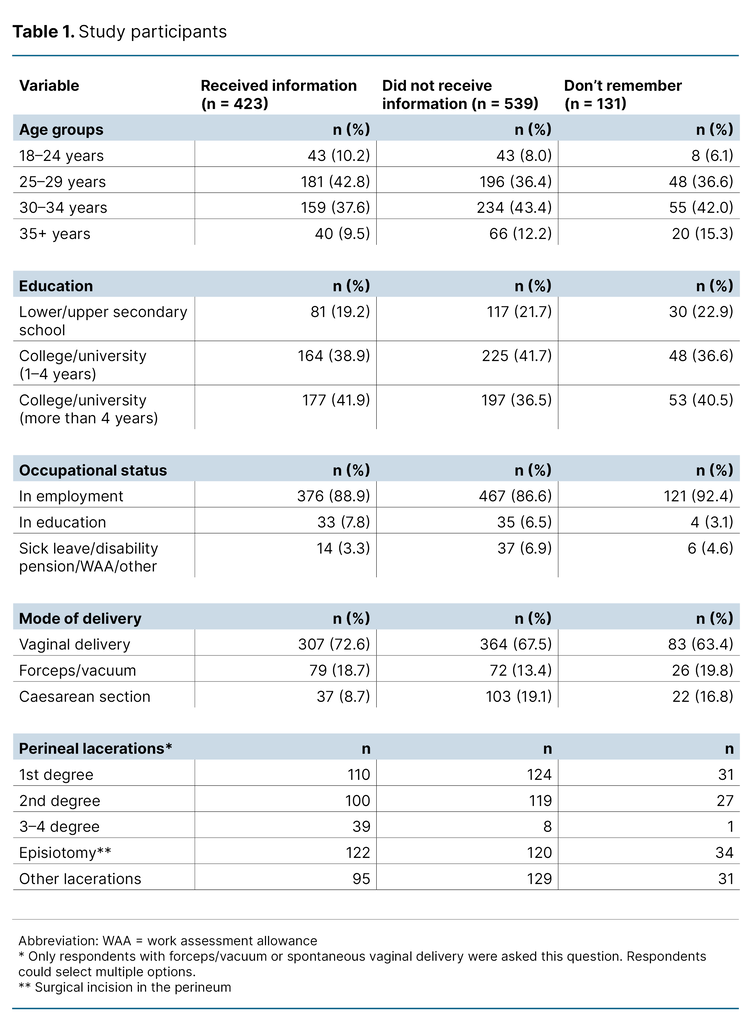
Ultimately, 1093 participants were included in the study, all of whom met the inclusion criteria and answered the subsequent questions. Table 1 summarises the characteristics of the study sample, stratified by whether participants received information on PFMT during the postnatal hospital stay.
Proportion of women who received information about PFMT during pregnancy and the postnatal hospital stay
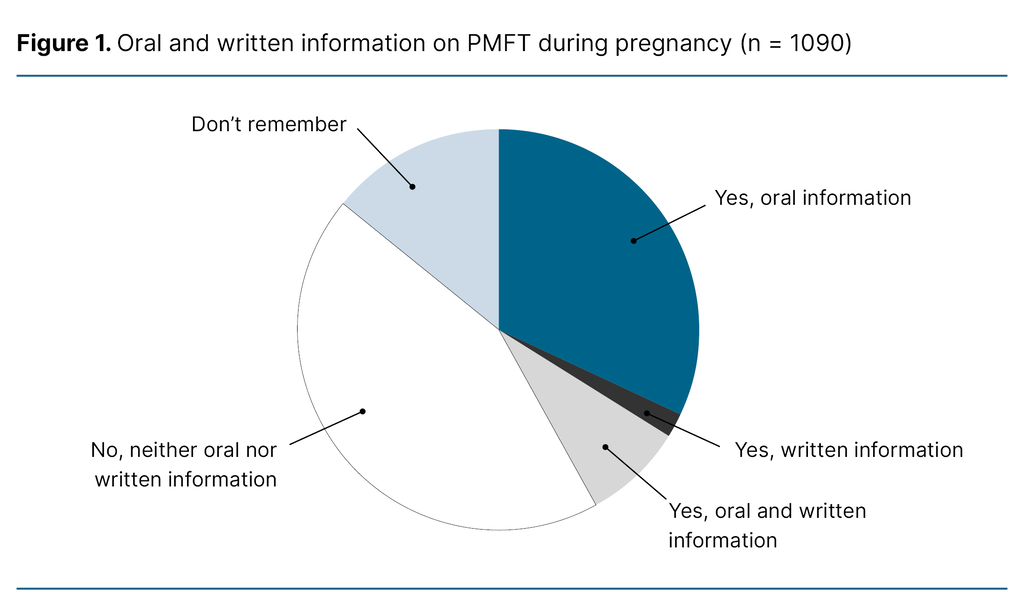
Figure 1 illustrates whether women received oral or written information about PFMT during pregnancy. At their antenatal consultations, just under half of the participants (44%) received neither oral nor written information. Among those who did receive information, most stated that it was provided orally (32%), while 2% received written information only.
A small proportion of women (8%) reported receiving both verbal and written information, while 14% did not remember whether they had received any information.
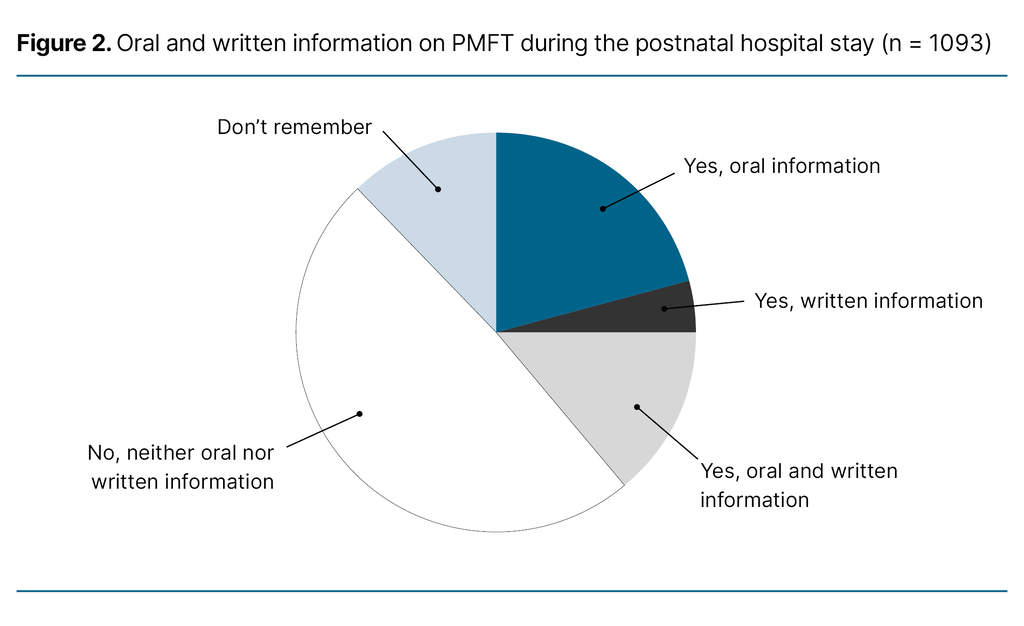
Figure 2 shows that nearly half of the respondents received neither oral nor written information (49%) during the postnatal hospital stay. Among those who received information, most received it orally (21%), while only a small proportion received written information (4%).
A few respondents indicated that they had received both oral and written information (14%). The remaining respondents (12%) could not recall whether they had received any information about PFMT during the postnatal hospital stay.
Type of information women received about PFMT and follow-up of pelvic floor function at the postnatal check-up
Study participants were asked what type of information they received at their postnatal check-up four to six weeks after giving birth. The most common topics addressed were sexual health and contraception (85%). Fewer than half reported that perineal lacerations and wounds were examined (44%), and about one-third indicated that PFMT was discussed (32%).
With regard to pelvic floor–related issues, the women reported that urinary leakage (13%), pelvic organ prolapse (10%), pelvic pain (9%) and leakage of gas or stool (5%) were discussed during the postnatal check-up.
Perceived adequacy of knowledge to maintain pelvic floor function based on information received and follow-up
Forty-two per cent of women reported that the information they received about PFMT during pregnancy, the postnatal hospital stay and at the postnatal check-up was adequate to some extent. Twenty per cent considered the information to be adequate to a large or very large extent. Over one-third of women felt that the information received during pregnancy was either completely inadequate or adequate to a small extent.
Four out of ten women considered the information received during the postnatal hospital stay to be adequate, while 25% reported receiving enough information to a large or very large extent. Most women rated the follow-up of pelvic floor function at the postnatal check-up as inadequate (68%), and only 12% considered it adequate to a large or very large extent.
Association between receiving information and maintaining pelvic floor function
Our findings show that the majority of participants attended the postnatal check-up (90%) and acquired knowledge about PFMT (86%) in order to maintain pelvic floor function. Most women reported that they did not contact healthcare personnel for further follow-up of pelvic floor function after the postnatal check-up (73%).
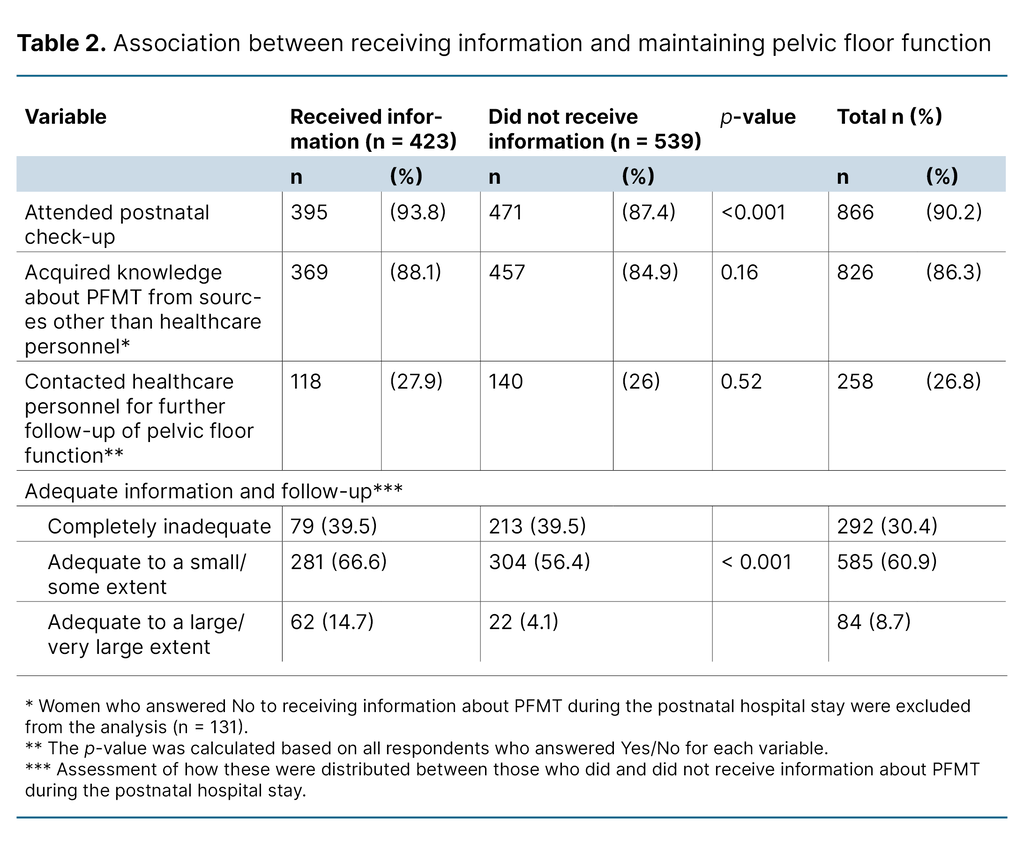
Table 2 presents the results of the correlation analysis comparing women who received information during the postnatal hospital stay with those who did not, as well as other information and follow-up variables. Associations between variables were assessed using Pearson’s chi-square test.
A significantly higher proportion of women who attended the postnatal check-up reported receiving information about PFMT during the postpartum hospital stay than those who did not attend the postnatal check-up.
There was no statistically significant association between whether women reported receiving information or not and whether they had acquired knowledge about PFMT from sources other than healthcare personnel (p = 0.16).
Likewise, no statistically significant association was observed between receipt of information and whether women contacted healthcare personnel for further follow-up of pelvic floor function (p = 0.52).
Participants were also asked whether they considered the information and follow-up regarding their pelvic floor to be adequate overall. A statistically significant association was found between receipt of information during the postnatal hospital stay and women’s assessment of whether the overall information and follow-up regarding pelvic floor function were adequate.
Discussion
The main findings of this study show that only 40% of respondents reported receiving information on PFMT during pregnancy and the postnatal hospital stay. Even fewer reported that PFMT was discussed at the postnatal check-up.
The information provided was inconsistent, and many women considered it inadequate to perform PFMT without further guidance. Most women acquired their own information and attended the postnatal check-up, but few contacted healthcare personnel for further follow-up.
Information on PFMT in antenatal and postnatal care
A large proportion of women reported not receiving any information on PFMT, either orally or in writing. Among those who did receive information, oral communication was most common. Parallel with our findings, a systematic review of findings from Sweden, Norway, the United Kingdom and Australia reported similar challenges, with women reporting a lack of adequate information on maternal health before, during and after childbirth (23).
National guidelines recommend that women receive information on PFMT during pregnancy, both to prevent pelvic floor issues and to facilitate postnatal training (1). Structured consultations during the postnatal hospital stay are also advised (2), but studies show that individualised guidance provides better outcomes than group sessions. Our findings indicate that these guidelines are not adhered to in practice.
Approximately one in ten women could not recall whether they had received information. Pregnancy and the postpartum period involve major hormonal changes, which, together with a new life situation and altered sleep patterns, can affect how receptive women are to information, according to Wiklund et al. (23). These findings highlight the need for tailored and repeated communication to ensure that information is understood.
Information and follow-up in antenatal and postnatal care
The information on PFMT varied considerably. While more than half of women received information on the importance of PFMT, fewer were given specific guidance on the timing and correct execution of exercises. Several studies show that PFMT during pregnancy can help prevent postnatal pelvic floor disorders (10, 11).
A study investigating the prevalence of pelvic floor disorders after childbirth reported that approximately one-third of women experienced urinary incontinence up to four years postpartum (7). The long-term impact of urinary incontinence is further highlighted in a study by Mendes et al. (24), in which women reported significant limitations in daily activities, social interactions and sexual intimacy, with some choosing to socially isolate themselves (24). These adverse outcomes could potentially be reduced through better information and follow-up.
Our findings showed that only about one-third of women reported receiving information during antenatal consultations on the recommended frequency and duration of pelvic floor exercises, with slightly fewer receiving this information during the postnatal hospital stay. Svenningsen and Maltau (25) emphasise that effective PFMT requires women to be aware of their pelvic floor muscles and to learn how to correctly activate them. Our results suggest, however, that women are often given inadequate information on this matter.
Few women also reported receiving an individualised pelvic floor exercise programme during the postnatal hospital stay. Evidence from multiple studies indicates that individualised follow-up with a physiotherapist yields better outcomes than unsupervised training (11, 13–15), and both Norwegian and British guidelines recommend exercise programmes tailored to each woman’s specific needs (2, 26).
Few women reported receiving information on pelvic floor symptoms that require follow-up by healthcare personnel. Without such information, women may be uncertain about what constitutes normal postpartum changes and when to seek medical advice. Although British guidelines recommend that women be informed about relevant symptoms, risk factors and treatment options (26), our findings suggest that these recommendations are not properly adhered to.
Women’s assessment of information received and follow-up by healthcare personnel
A large proportion of women in our study reported that the information they received during antenatal and postnatal care was insufficient to enable them to perform PFMT. Our findings contrast somewhat with national data on user experiences with antenatal, intrapartum and postnatal care (PasOpp reports).
These surveys do not specifically examine information on PFMT or follow-up of pelvic floor function, but they are among the few national studies capturing women’s experiences related to pregnancy and childbirth. Unlike our study, which found only minor differences between antenatal and postnatal care, the PasOpp reports indicate that women were more satisfied with the information received during pregnancy than during the postnatal period (27, 28).
A similarity with our findings is that women reported being least satisfied with the information received during the postnatal check-up at the child health centre (28). One possible explanation for why participants in our study reported lower satisfaction with information at the postnatal check-up is that they were asked specifically about PFMT, whereas the PasOpp reports address physical health more broadly.
Our findings are consistent with international studies showing that women consider information on pelvic floor health to be inadequate (29–32). This can have long-term negative consequences for women’s health and quality of life. It is therefore essential to strengthen the provision of information and ensure that recommended guidelines are adhered to in practice.
It is also worth noting that the national guidelines for postnatal care (2) have not been revised since 2014. Our findings indicate there is room for improvement in the information and follow-up women receive. Any future revision should consider the poor adherence to current recommendations and assess the feasibility of implementing individualised follow-up.
Reflections on methodology
Recruitment via social media provided rapid access to relevant participants and yielded a high response rate. The cross-sectional study included a broad sample and examined potential associations between numerous variables. The statistical analyses provided a basis for assessing how the information received and follow-up may have shaped women’s perceptions of the information they received about PFMT.
The study has several limitations. The cross-sectional design prevents any conclusions being drawn about causal relationships (33). Our sampling method may have introduced selection bias, as participation was self-selected. Women without access to social media or with language barriers are likely to be underrepresented. This bias could result in the study sample appearing more satisfied with follow-up than the general population, thereby limiting external validity (33).
Another limitation is that we did not account for potential confounding factors in the correlation analyses, such as education level or social support, which may have impacted on the results. For example, women with a higher education may be better positioned to seek information and contact healthcare services regardless of what information is provided during the postnatal hospital stay.
Furthermore, the study is based on self-reported data, which carries a risk of recall bias. We attempted to reduce this by only including women who had given birth within a limited time frame. Self-reported data can also introduce information bias if participants are reluctant to report personal details or if they select responses they consider to be socially desirable. Additionally, the self-developed survey questions may have introduced further information bias if participants misunderstood them or interpreted them differently.
Sociodemographic data indicate that our sample largely reflects the general population. The largest proportion of participants were aged 30–34 years, which is consistent with the mean age of first-time mothers in Norway of 30.2 years (34).
However, 5.7% of our sample reported experiencing a third or fourth-degree perineal laceration, compared with 2.7% reported by the Norwegian Institute of Public Health (35). Women with more severe perineal injuries may be more interested in the topic of this study, which could explain the difference in proportions. While this provides some degree of generalisability, the findings should be interpreted with caution due to methodological limitations.
Implications for clinical practice
Based on the information received by our study participants, improvements are needed in the information provided on PFMT and the follow-up of pelvic floor function during antenatal and postnatal care. This could be addressed through training programmes for healthcare personnel, enabling them to update their knowledge on the pelvic floor and its role in the prevention and management of pelvic floor–related disorders. Training should also incorporate findings from this study to ensure that the content is relevant and founded on women’s experiences.
The findings should be used to inform various groups of healthcare personnel about the importance of informing and instructing women on the role of PFMT during pregnancy, after childbirth and for the rest of their life, as well as the current gaps in such information.
A focus on how pelvic floor exercises should be performed in practice before and after childbirth can also help ensure that more women receive adequate information to do so. Follow-up with a physiotherapist in the public health service is also an alternative, and this could facilitate the early identification of pelvic floor–related problems and ensure women receive adequate information and follow-up.
Conclusion
Few women reported receiving information on PFMT during pregnancy, the postnatal hospital stay, or at the postnatal check-up. Insufficient follow-up can have serious consequences for women’s health and quality of life. Although many women sought information independently and attended postnatal check-ups, few contacted healthcare personnel for further follow-up.
The findings indicate a need for individualised follow-up by healthcare personnel, such as publicly funded physiotherapy integrated into postnatal care. The study also highlights a mismatch between national guidelines and women’s experiences.
The authors declare no conflicts of interest.
Open access CC BY 4.0
The Study's Contribution of New Knowledge

Comments