Caring for children in the general intensive care unit – the experiences of intensive care nurses
Summary
Background: Intensive care nurses in general intensive care units must care for patients of all ages. Most Norwegian hospitals do not have a dedicated paediatric intensive care unit. Thus, acutely and critically ill children are cared for in the general intensive care unit, where there is a majority of adult patients. The children are in a particularly vulnerable situation. Their diagnoses and illnesses often differ from those of critically ill adult patients.
Objective: To acquire insight into the perceptions and experiences of intensive care nurses when caring for acutely and critically ill children admitted to the general intensive care unit.
Method: We used a qualitative, exploratory design. Two qualitative focus group interviews were conducted with altogether ten intensive care nurses employed in the general intensive care unit. A phenomenological hermeneutic research method was adopted. We analysed the data material using Graneheim and Lundman’s qualitative content analysis.
Results: The analysis identified three themes: good preparation leads to safe treatment, cooperation in the child’s best interests, and relating to children according to their development stage. Each theme is illustrated by three to five categories.
Conclusion: The study shows that the intensive care nurses generally felt positive about caring for children in the general intensive care unit, even though they had experienced feelings of insecurity and unease. Measures such as good training, good cooperation and fulfilling the child’s needs had enhanced their experiences.
Cite the article
Gravdal H, Sandnes H, Gundersen E. Caring for children in the general intensive care unit – the experiences of intensive care nurses . Sykepleien Forskning. 2020;15(80265):e-80265. DOI: 10.4220/Sykepleienf.2020.80265en
Intensive care nurses (ICU nurses) take care of acutely and critically ill patients of all ages and ensure a sound professional provision of treatment (1, 2). The term ‘acutely and critically ill’ indicates that the condition is, or can become, life-threatening if it is not treated (3).
Children in the intensive care unit (ICU) are in a particularly vulnerable situation (4). The diagnoses and illnesses of critically ill children often differ from those of adult patients (5, 6). Children are in a continuous process of development, and ICU nurses must adapt to their development stage (7).
The majority of Norwegian hospitals do not have a dedicated paediatric ICU. Thus, children in need of intensive care are admitted to a general ICU (8). When children are treated in the ICU, this affects the whole family, and the children need to have their parents at the hospital (9, 10). Nursing should be centred around the whole family, not only the sick child (10, 11).
Many challenges are encountered in treating children in units with a majority of adult patients (5). Intensive care nurses in a general ICU do not have the same expertise in treating children as in the case of adults.
Normally, they have less understanding of and knowledge about paediatric patients, and this may create anxiety and uncertainty. In addition, many of them have greater compassion for children and often have children of their own to relate to (12).
Objective of the study
We have not found any studies describing how ICU nurses experience caring for acutely and critically ill children in a general ICU. Consequently, there is a need for new knowledge adapted to the child’s specific needs for treatment and care.
The objective of the study is to gain insight into the perceptions and experiences of ICU nurses in their encounters with this group of patients. We formulated the following research question: How do intensive care nurses experience caring for acutely and critically ill children in the general ICU?
Method
We used a qualitative, exploratory design. A qualitative approach is suited to examining processes such as interaction, development, movement and the overall picture (13). One and the same reality can be described from different perspectives. The goal is to explore meaning content in social and cultural phenomena as perceived by those involved (14).
Two focus group interviews with intensive care nurses from the same general ICU were conducted. The focus group interview is appropriate when wishing to explore phenomena that relate to common experiences, attitudes or views in an environment with interaction among many people (14, 15).
We used a phenomenological hermeneutic approach. This identifies lived experience by describing people’s experiences and then interpreting the data material by extracting the essence of the text and arriving at the main concepts of lived experience (16). The essential meaning is studied and revealed in the interpretation of the transcribed text (17).
Sample
The inclusion criteria for participation were as follows: intensive care nurse employed at a general ICU that treats children. The informants were required to be working at least 75 per cent of a full time equivalent as a minimum, and to have been responsible for the nursing care of children admitted to the unit in order to ensure that they had experience of this patient group.
Members of the children’s resource group in the unit were excluded since they probably had more knowledge and experience of this group of patients than the majority of the staff. The sample consisted of ten female ICU nurses aged 31–54 years with experience ranging from 6 months to 20 years from a general ICU. Seven of the informants had children of their own.
The study was approved by the Norwegian Centre for Research Data (NSD, reference number 50826) and by the hospital’s data protection officer prior to the interviews. The informants signed a consent form and were informed that they could withdraw from the study at any time.
Data collection
After carrying out a pilot interview, we conducted two focus group interviews in December 2016 and January 2017. This is in line with Malterud (14), who recommends two groups as a starting point for data collection. Five informants took part in each interview, which lasted approximately one hour. The number of informants in each group was based on the recommendations in the literature on research methodology (18).
The interview guide contained a small number of open-ended questions organised under three main themes: experiences, sense of mastery and potential for improvement. We chose an open structure with little moderator intervention. We concentrated on the informants’ discussion with each other rather than requesting them to answer specific questions.
All the informants engaged in a good dialogue and were active in the conversation. They described the phenomena in their own words. The first author was the moderator and ensured that the conversation covered the themes of interest. We had prepared follow-up questions, but there was no need to use these.
The second author was present during both interviews. She noted facial expressions and the general atmosphere and had the opportunity to add comments. We thereby ensured that there was agreement between non-verbal language and verbal language.
The interviews were audio-recorded and transcribed straightaway. The data material provided rich descriptions. There was no need for supplementary interviews (14).
Analysis
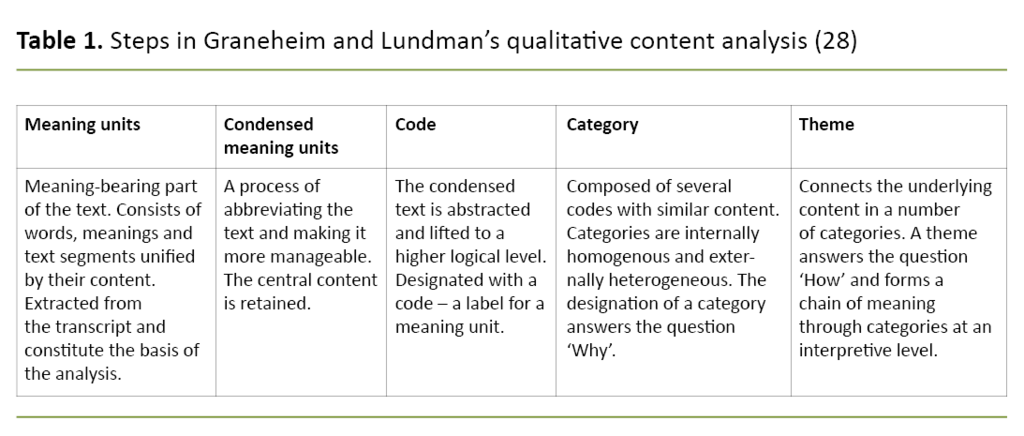
The data analysis was performed using Graneheim and Lundman’s (19) qualitative content analysis with an inductive approach. The method encourages descriptions of the manifest content of the text and interpretation of the latent message (20). This is in accordance with a phenomenological hermeneutic research design.
The transcribed material was first read in its entirety. The first and second authors then separately identified meaning units in the text. The meaning units were condensed into a higher level of abstraction prior to being coded (Table 1).
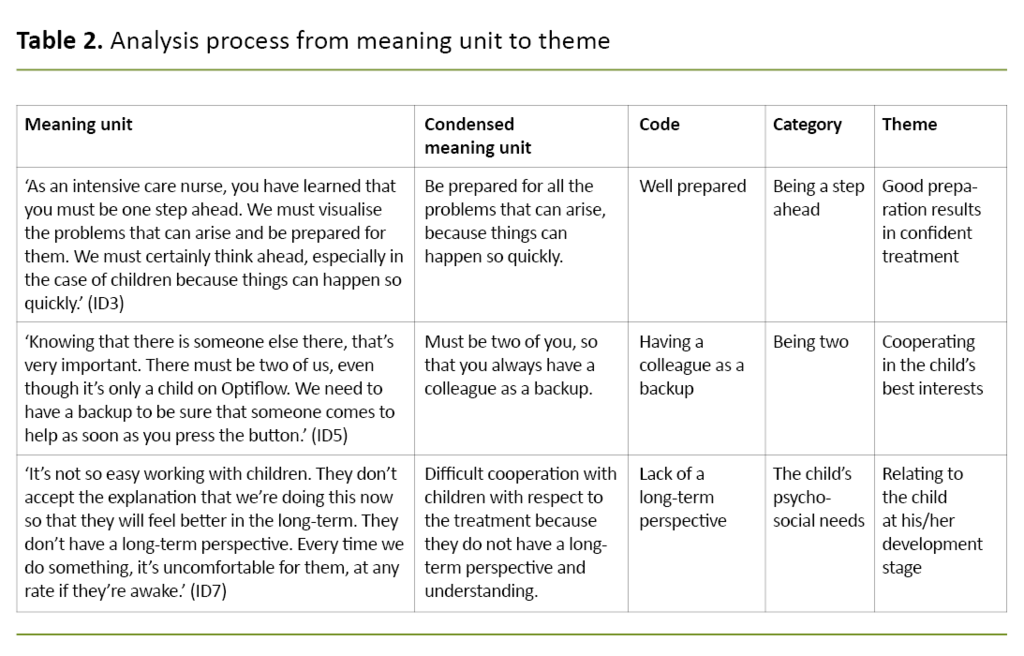
The further analysis of codes and categories leading to the themes was discussed by the authors until agreement was reached (Table 2).
Results
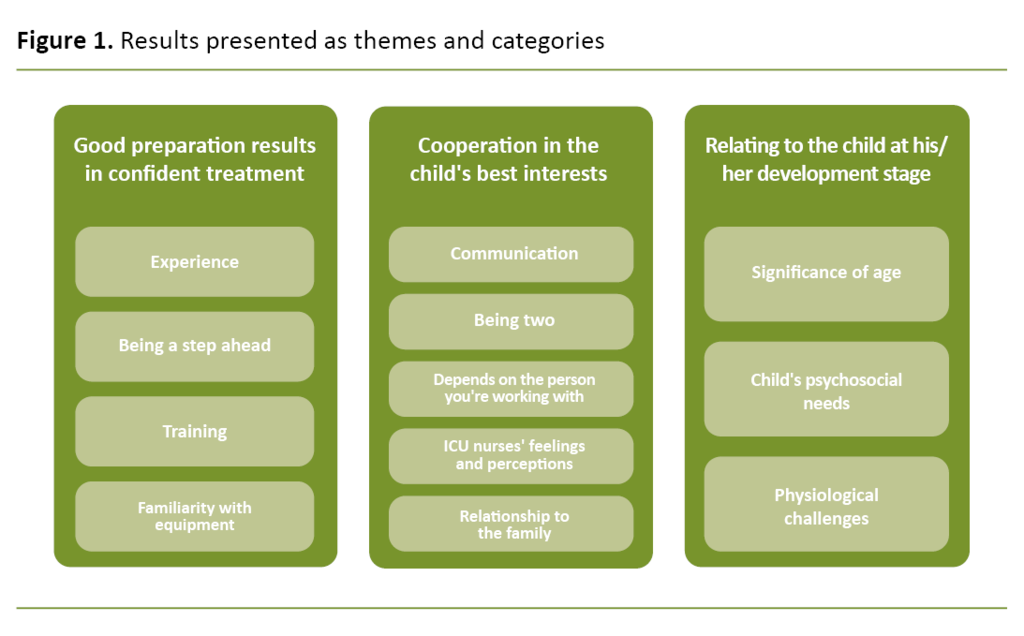
We identified three themes. Each theme consisted of from three to five categories (Figure 1).
Good preparation results in safe treatment
The informants emphasised the importance of having experience of the patient group. One informant said the following: ‘I think a lot of the uncertainty that prevails when a child is admitted is because we have too little experience of this.’ (ID5)
It felt easier having responsibility for an acutely and critically ill child if they had experienced this a few times before: ‘I notice that I’m gradually acquiring more experience and composure, and that actually feels quite good.’ (ID8)
The informants wanted new ICU nurses to be given a chance to participate: ‘People must be given a chance so that it’s not always the same ones who are assigned to children. That’s how you build experience.’ (ID10)
All the informants said that it was important to be mentally prepared to work with children. If they had imagined the worst-case scenario and had thought about possible solutions, they were well prepared.
The ICU has a form to be completed in cooperation with the doctor that provides an overview of drugs and equipment that a child requires if there is a need for intubation. The informants found this form very reassuring. One said the following: ‘Having the form raises my confidence enormously because you know what you are to administer, and what equipment you should have.’ (ID2).
Good reference books and updated procedures in relation to children were highlighted as important for being well prepared. The informants stressed the importance of good training.
Having more simulations was a suggested improvement.
The unit’s resource group for children was highly esteemed: ‘I’m very happy we have the children’s resource group, and they hold a practical training session once a year. That’s one of the most useful measures.’ (ID1)
Some informants thought that nurses would feel more confident if certification were required for working with children. Having more simulations was a suggested improvement. Several informants proposed introducing secondment to the paediatric department in order to experience an environment with only children.
It was easier to remain calm in relation to having responsibility for a child if the ICU nurses were familiar with the equipment and mastered its use. Everyone agreed that it was vital to be able to rely on the equipment. One of the biggest challenges was to know what equipment to use with regard to the child’s age and size.
Several informants suggested that the individual ICU nurse should assume more responsibility for practising connecting the child’s ventilator and checking the critical care trolley with special equipment for children. Management must set aside time for practice and make provision for teaching and training in the unit.
Cooperation in the child’s best interests
All the informants talked a lot about the importance of good cooperation between colleagues, and with the family members and with the child. Good communication was stressed as playing a decisive role. It was very stressful when the doctors did not listen to the concerns of the ICU nurses.
All the informants believed it was important to have a joint plan and clear communication. One informant stated the following about a confused situation when many people were present in the room: ‘Instructions were given fairly clearly, but who was it who actually took responsibility for carrying out the instructions? (ID9)
The informants emphasised how important it was that there was acceptance for feeling less confident when treating children, and that colleagues were backed up and supported.
They also thought it important that there should be two ICU nurses when caring for a child. Knowing that a colleague was always available and having someone with whom to exchange experiences and knowledge, boosted their confidence: ‘It’s not always about needing an extra pair of hands but two brains are better than one.’ (ID3)
Clear task distribution was important. One ICU nurse could sit with the child to make sure that the child did not pull out its ventilation tube, while the other could deal with the paperwork, medication and other tasks.
How the ICU nurses perceived the task of caring for children depended on whom they were working with; ‘The more confident you are about the other person, the more secure you feel about having responsibility for a child.’ (ID6)
The informants described working with stressed colleagues as unpleasant. Several said that they often felt it was easier to work with less experienced ICU nurses because they did not act as if ‘they knew it all’.
Having extensive experience did not necessarily mean that they remained calm in stressful situations. Nevertheless, several informants stated that they were uncomfortable if the other person was very inexperienced. Some colleagues gave the impression of distrust and were monitoring what you were doing.
In stressful situations, several informants had experienced a feeling of being misunderstood, and that disparaging remarks were thrown around. Such incidents were particularly challenging if the child’s parents were present.
Creating a good relationship with parents and family members was important. The distribution of responsibility vis-à-vis the child had to be clarified with the parents. The aim was for the parents to entrust professional and medical responsibility to intensive care nurses and concentrate solely on being parents: ‘They’re the ones who know the child best, and it’s extremely important to listen to them. At the same time, we are the ones with the professional responsibility.’ (ID3)
Family members influenced the atmosphere in the room, and it was vital to be able to calm them down.
The informants expressed mixed feelings about having responsibility for children. The child’s prognosis was the deciding factor and several informants said that the more serious the prognosis, the more difficult it became. A bad gut feeling resulted in greater mental stress.
In situations where they had been substantially involved with a critically ill child, it could be painful to break away and pass on the responsibility. Many were also anxious about making mistakes with fatal consequences.
Relating to the child at his/her development stage
Opinions were mixed as to whether the age of the child had any bearing on how intensive care nurses experienced caring for the child in the ICU. Some informants felt caring for the youngest children was most difficult, since their anatomies are smaller.
Some informants felt that children aged 3–4 years were the most challenging because they could be uncooperative. A few informants thought that children bordering on adulthood were most challenging. Yet others felt this was safer because the older children had a greater physiological reserve capacity.
The physiological differences between children and adults could be challenging. Several informants had found that children were more quickly exhausted because of a smaller reserve capacity.
The physiological differences between children and adults could be challenging.
Administering medication was more difficult because of unaccustomed dosages and higher metabolism in children. Nevertheless, everyone agreed with the informant who said as follows: ‘We know what we must do. The treatment principles are the same. It’s just that the format is smaller.’ (ID6)
The informants said that communication with children could be challenging. One informant said: ‘I find it difficult because children in these situations regress. How clear and honest can you be? Should you sugar-coat it? Should you baby talk?’ (ID7)
Several of the informants found that the children appeared to be frightened, and that it was difficult for them to be in unfamiliar surroundings. The ICU nurses felt it was important to focus on the child and keep him/her calm. One of the informants said the following: ‘You have to calm the child. If not, they’ll use up their reserves, and they don’t have a lot to go on.’ (ID10)
A number of informants felt it was traumatic for small children with many strangers and it was therefore important to limit the number of people in the room.
Discussion
ICUs that deal with both adults and children face many challenges. The study shows that the degree of preparation is crucial for how the intensive care nurses experience caring for children. The informants found that if they were prepared for the situations that might occur, they felt that they had more control.
The informants wanted to have in-service training days and simulations
Little experience of the patient group was the source of considerable insecurity, and good training was deemed important. Offord (5) recommends that general ICUs have an educational strategy that includes a paediatric in-service training day. This will strengthen the ICU nurses’ knowledge, skills and confidence when caring for acutely and critically ill children.
The informants wanted to spend time working in a paediatric unit to improve their knowledge.
The informants in our study had an annual in-service day devoted to skills and procedures training together with the children’s resource group. They wanted more time to be set aside for this, and also wanted more simulations. Simulation-based team training in one’s own unit increases confidence in one’s own skills and helps to enhance the quality of patient treatment (21).
Simulations can be carried out in all ICUs. The informants wanted to spend time nursing in a paediatric unit to improve their knowledge. ICU nurses who lack experience of caring for children can be given training in order to increase their knowledge of the patient group (22, 23).
Intensive care units need training and good collaboration
Vanore (12) points to the differences between children and adults as patients, drawing attention to how important it is to ensure that the staff are well educated and trained. The informants in our study were eager that provision should be made for good training in the unit. They wanted time to be set aside so that they could familiarise themselves with the equipment and instruments.
Familiarity with ICU equipment is important in intensive care nursing, particularly in situations characterised by stress and unpredictability. Such familiarity is achieved when the ICU nurse is able to concentrate on the patient at the same time as he or she manages the equipment on which the patient is dependent (3).
The informants in the study pointed out that collaboration with the team around the child was vital. Good cooperation depended on who they worked with and how they communicated with each other. According to Siffleet et al. (24), good teamwork positively affects the emotional wellbeing of intensive care nurses and the ICU environment.
If intensive care nurses are not confident that a colleague can perform the work, it can lead to stress and agitation and a feeling of having to do the other person’s job (10).
Several of the findings in our study are similar to Rall and Dieckmann’s (25) principles for dealing with and avoiding acute crises in the hospital environment. Crisis Resource Management (CRM) has the aim of coordinating, utilising and employing all available resources to provide the best possible patient treatment.
Important main principles in our study that CRM also highlights are knowing the environment, drawing up a plan, having a satisfactory work allocation and effective communication. Our informants emphasised the importance of these principles.
A calm atmosphere allowed the informants to cope with stress
Team performance is strengthened if team members know how the team reacts in acute situations (26). The informants in our study found that it was vital that two ICU nurses shared responsibility for a child. The doctors were highlighted as an important part of the team around the patient.
The informants were reliant on good cooperation and that they could talk to each other in a pleasant and polite tone. Colleagues who were able to calm down and retain their composure in stressful situations were preferred as partners.
If the informants managed to create a pleasant, calm atmosphere around the patient, they gained a greater feeling of mastery from caring for children. The intensive care nurse’s personal qualities impact on the parents’ ICU experience (9). Our informants were focused on good cooperation with the children’s parents and regarded them as a nursing resource.
ICU nurses can help to alleviate the disagreeable experience for the patient by including family members as a resource (27). They are not only treating the child but the entire family as a collective unit around the sick child (6, 10).
All the child’s needs must be fulfilled
The informants focused on fulfilling all the needs of the child, both physical and psychosocial. Findings in the study of Mattson et al. (4) confirm this and show the importance of holistic nursing. Acutely and critically ill children are in a particularly vulnerable situation and depend on the ICU nurses to understand their needs (4, 7).
Our informants often found communication with the children challenging.
Our informants were fully aware that children differ from adults and considered their smaller anatomic reserve capacity and higher metabolism as particular challenges. Robb (16, 17) also identifies the same challenges. He claims that the physical differences between children and adults are one of the greatest concerns of intensive care nurses when caring for children.
Our informants often found communication with the children challenging. Good communication is vital in reducing stress in connection with medical treatment and the problems the ICU environment creates for the patient (27).
Discussion of method
The research in this study was carried out in the authors’ own field of expertise. This may have coloured the findings. At the same time, this was a strength in understanding the data material. The first author was the moderator in both interviews. She had no experience of nursing children, which in our assessment would minimise the risk of our preconceptions influencing the informants.
According to Graneheim et al. (28), one must ask whether the results are true, stable and relevant in order to elucidate different aspects of the study’s credibility. The researchers’ responsibility is to provide sufficient descriptive data so that the reader can assess whether the findings can be transferred to a different context (29).
The credibility of our study is strengthened by quotes from the informants and the inclusion of tables and figures. The spread in the informants’ age, their experience from the general ICU and the fact that we included informants with and without children of their own serve to strengthen the study’s credibility and transferability.
A weakness may be that all informants are female, but this reflects the skewed gender balance in the ICU. The interviews were conducted at a general ICU, and the findings can therefore not be generalised to apply to all intensive care units because of differences in the structure and staffing of the units.
Nevertheless, there is reason to believe that our findings have adequate information value, taking into account the objective, sample, theory, quality of data and method of analysis (30), and may be transferable to units with a similar structure.
Further research can help provide key knowledge and greater awareness of the challenges linked to ICUs that treat both children and adults. An observation study could provide supplementary information that does not emerge in a focus group interview. A study of the experiences of intensive care nurses before and after the implementation of measures such as in-service training days, may prove useful.
Conclusion
The study shows that intensive care nurses generally considered caring for children in a general ICU to be a positive experience even though they had also felt uncertain and insecure. Measures such as good training and cooperation, and the feeling that they were fulfilling the child’s needs enhanced their experience.
References
1. Norsk Sykepleierforbund. Funksjons- og ansvarsbeskrivelse for intensivsykepleiere. Available at: https://www.nsf.no/Content/3653453/cache=1512504484000/FA_intensivsykepleiere.pdf. 2017 (downloaded 11.04.2018).
2. Utdannings- og forskningsdepartementet. Rammeplan for videreutdanning i intensivsykepleie. Oslo; 2005. Available at: https://www.regjeringen.no/globalassets/upload/kilde/kd/pla/2006/0002/ddd/pdfv/269388-rammeplan_for_intensivsykepleie_05.pdf (downloaded 26.04.2018).
3. Moesmand AM, Kjøllesdal A. Å være akutt kritisk syk: om pasientenes og de pårørendes psykososiale reaksjoner og behov. 2nd ed. Oslo: Gyldendal Akademisk; 2004.
4. Mattsson J, Forsner M, Castrén M, Arman M. Caring for children in pediatric intensive care units: an observation study focusing on nurses' concerns. Nursing Ethics. 2013;20(5):528–38.
5. Offord RJ. Caring for critically ill children within an adult environment – an educational strategy. Nursing In Critical Care. 2010;15(6):300–7.
6. Endacott R. Needs of the critically ill child: a review of the literature and report of a modified Delphi study. Intensive and Critical Care Nursing. 1998;14:66–73.
7. Coetzee M, Britton M, Clow SE. Finding the voice of clinical experience: participatory action research with registered nurses in developing a child critical care nursing curriculum. Intensive and Critical Care Nursing. 2005;21:110–8.
8. Norsk anestesiologisk forening og Norsk Sykepleierforbunds landsgruppe av intensivsykepleiere. Retningslinjer for intensivvirksomhet i Norge. Oslo; 2014. Available at: https://www.nsf.no/Content/2265711/Retningslinjer_for_IntensivvirksomhetNORGE_23.10.2014.pdf (downloaded 17.10.2019).
9. Sjuls M, Johannessen B. Foreldres opplevelser i intensivavdelingen. Sykepleien Forskning. 2015;10(3):248–55. DOI: 10.4220/Sykepleienf.2015.55027
10. Mahon PR. Acritical ethnographic look at paediatric intensive care nurses and the determinants of nurses’ job satisfaction. Intensive and Critical Care Nursing. 2014;30(1):45–53.
11. Foster JM, Whitehead L, Maybee, P, Cullens V. The parents’, hospitalized child’s, and health care providers' perceptions and experiences of family centered care within a pediatric critical care setting: a metasynthesis of qualitative research. Journal of Family Nursing. 2013;19(4):431–68.
12. Vanore ML. Care of the pediatric patient with brain injury in an adult intensive care unit. Critical Care Nursing Quarterly. 2000;23(3):38–48.
13. Barroso J. Qualitative approaches to research. In: LoBiondo-Wood G, Haber J, eds. Nursing research: methods and critical appraisal for evidence-based practice. 7th ed. St. Louis, Missouri: Elsevier Mosby; 2010. s. 100–26.
14. Malterud K. Fokusgrupper som forskningsmetode for medisin og helsefag. Oslo: Universitetsforlaget; 2012.
15. Barbour RS, Kitzinger J. Developing focus group research: politics, theory and practice. London: Sage; 1999.
16. Polit D, Beck CT. Nursing research. Generating and assessing evidence for nursing practice. London: Lippincott, Williams & Wilkins; 2012.
17. Lindseth A, Norberg A. A phenomenological hermeneutical method for researching lived experience. Scandinavian Journal of Caring Sciences. 2004;18(2):145–53.
18. Wibeck V. Fokusgrupper: om fokuserade gruppintervjuer som undersökningsmetod. Lund: Studentlitteratur; 2011
19. Graneheim UH, Lundman B. Qualitative content analysis in nursing research: concepts, procedures and measures to achieve trustworthiness. Nurse Education Today. 2004;24(2):105–12.
20. Lundman B, Graneheim UH. Kvalitativ innehållsanalys. I: Granskär M, Höglund-Nielsen B. Tillämpad kvalitativ forskning inom hälso- och sjukvård. Lund: Studentlitteratur; 2012.
21. Rød I, Moen WEI, Struksnes S. Simuleringbasert teamtrening på barneavdeling. Sykepleien Forskning. 2017;12(61032):(e-61032). DOI: 10.4220/Sykepleienf.2017.61032
22. Robb JA. Caring for children in an adult intensive care unit. Part I. Intensive & Critical Care Nursing. 1995;11(2):100–10.
23. Robb JA. Caring for children in an adult intensive care unit. Part 2. Intensive & Critical Care Nursing. 1995;11(3):161–9.
24. Siffleet J, Williams AM, Rapley P, Slatyer S. Delivering best care and maintaining emotional wellbeing in the intensive care unit: the perspective of experienced nurses. Applied Nursing Research. 2015;28(4):305–10.
25. Rall M, Dieckmann P. Errors in medicine, patient safety and human factors. Wien: European Society of Anaesthesiology; 2005. Available at: https://www.guysandstthomas.nhs.uk/resources/education-training/sail/reading/crisis-mgt-pt-safety.pdf (downloaded 17.10.2019).
26. Ballangrud R, Hall-Lord ML, Persenius M, Hedelin B. Intensive care nurses' perceptions of simulation-based team training for building patient safety in intensive care: a descriptive qualitative study. Intensive & Critical Care Nursing. 2014;30(4):179–87.
27. Kolloen K. Intensivsykepleie. Pasienter på intensiv trenger oppfølging. Sykepleien. 2011;99(7):55–57. DOI: 10.4220/sykepleiens.2011.0105
28. Graneheim UH, Lindgren BM, Lundman B. Methodological challenges in qualitative content analysis: a discussion paper. Nurse Education Today. 2017;(56):29–34.
29. Lincoln YS, Guba EG. Naturalistic inquiry. Beverly Hills, California: Sage; 1985.
30. Malterud K, Siersma VD, Guassora AD. Sample size in qualitative interviews studies: guided by information power. Qualitative Health Research. 2016;26(13):1753–60.
Comments